Omega-6
now browsing by category
‘Long Vax’ Finally Enters Lexicon
Reproduced from original article:
https://articles.mercola.com/sites/articles/archive/2024/04/05/covid-vaccine-long-vax.aspx
Analysis by Dr. Joseph Mercola April 05, 2024

Story at-a-glance
- Dr. Pierre Kory and Dr. Paul Marik are trying to get the word out that long vax is not only real but has disabled many Americans who were at the peak of health prior to getting a COVID jab
- At Kory’s long COVID clinic, 70% of the patients actually have long vax and reported their symptoms began “minutes, hours, days or several weeks” after receiving a COVID-19 shot
- Long vax symptoms are nearly identical to those of long COVID — the difference being that the long vax patients tend to be sicker, with more frequent small fiber neuropathy and dysautonomia
- A study by Yale scientists detailed long vax, which they called chronic post-vaccination syndrome, in 241 people
- Top reported symptoms include exercise intolerance, excessive fatigue, numbness, brain fog and neuropathy
An estimated 6.4% of U.S. adults have experienced symptoms of long COVID, a term used to describe a complex disorder that persists for three or more months after contracting COVID-19.1 While long COVID has been extensively covered in the media, millions more suffer from long vax — a condition with nearly identical symptoms to long COVID, but often even more severe.
New York pulmonologist Dr. Pierre Kory and Dr. Paul Marik, a critical care doctor formerly with Sentara Norfolk General Hospital in East Virginia, are part of the Front Line COVID-19 Critical Care Working Group (FLCCC). They’re trying to get the word out that long vax is not only real but has disabled many Americans who were at the peak of health prior to getting a COVID jab.2
At Long COVID Clinic, 70% of Patients Have Long Vax
Kory opened a tele-health practice that specializes in treating COVID disease, including long COVID. Kory says:3
“Long COVID, although a new name, is not a new disease. It meets the diagnostic criteria for a decades-old condition called myalgic encephalitis/chronic fatigue syndrome (ME/CFS).
The three symptom ‘pillars’ which lead to the diagnosis are fatigue, post-exertional malaise (PEM), and ‘brain fog’ (i.e. cognitive deficits ranging from word finding difficulties, short term memory loss, inability to focus/comprehend, and more rarely confusion or disorientation).
Although this triad is present in nearly every patient I see (rarely brain fog is missing), the patients also present with a ‘side menu’ of problems which can include sensory neuropathies, dysautonomia/POTS, motor neuropathies, abdominal issues, musculoskeletal complaints, and cranial symptoms (i.e tinnitus, vertigo, headaches, vision, hearing loss, smell loss, taste loss).
Many of my patients are debilitated and meet criteria for disability, despite the majority reporting being in the peak of health and functioning prior to the pandemic.”
Yet, Kory and colleagues quickly noticed that most of their patients reported their symptoms began “minutes, hours, days or several weeks”4 after receiving a COVID-19 shot. While many had also had COVID-19, only a small number tied their symptoms to the viral infection.
While the team initially called the condition post-COVID vaccine injury syndrome, they changed the diagnosis to “long vax” because the symptoms were so close to long COVID — the difference being that the long vax patients tended to be sicker, with more frequent small fiber neuropathy and dysautonomia, Kory said.5
Research Details Neuropathic Symptoms Following COVID-19 Jabs
Scientific studies detailing long vax symptoms continue to emerge. In one study from early in the pandemic, more than two-thirds of those reporting long COVID symptoms had negative antibody tests, suggesting at least some of them didn’t even have COVID-19.6 Meanwhile, many COVID jab recipients report long COVID-like symptoms.
As reported by Science magazine in 2022, “In rare cases, coronavirus vaccines may cause long COVID-like symptoms,”7 which can include (but is not limited to) brain fog, memory problems, headaches, blurred vision, loss of smell, nerve pain, heart rate fluctuations, dramatic blood pressure swings and muscle weakness. The feeling of “internal electric shocks” are also reported.
Also in 2022, a preprint study from the U.S. National Institutes of Health reported new neuropathic symptoms that began in 23 adults within one month of receiving a COVID-19 shot.8 All of the patients felt severe tingling or numbness in their faces or limbs, and 61% also experienced dizziness when standing up, intolerance to heat and heart palpitations.
When 12 of the patients had their nerve function tested, seven had less sweating in their hands and feet than normal, while six had a condition where their heart beats too fast when they stand up.9
The researchers also took skin samples from the lower legs of 16 patients. Among them, 31% showed signs that the small nerves in the skin were not as dense as they should be, which can indicate nerve damage. Another 13% were on the border of being considered damaged, and 19% had swollen nerve fibers. When five of the samples were evaluated more closely, signs of an immune reaction in the blood vessels were detected.10
Further, while electrical tests on the nerves were normal for most participants, 52% showed clear signs of damage to the small nerves that can be felt but not easily seen. The study shows that after getting the COVID-19 shot, a range of symptoms related to nerve damage is possible, which might be caused by an immune system reaction.

Save This Article for Later – Get the PDF Now
Yale Scientists Detail Long Vax Symptoms
A study by Yale scientists, including Dr. Harlan Krumholz of Yale School of Medicine in New Haven, Connecticut, also shed light on long vax, which they described as chronic post-vaccination syndrome, or PVS.11 In a study of 241 people who reported PVS after an mRNA COVID-19 shot, the median time from the jab to the onset of symptoms was three days, with symptoms continuing for 595 days. The five most common symptoms included:12
- Exercise intolerance (71%)
- Excessive fatigue (69%)
- Numbness (63%)
- Brain fog (63%)
- Neuropathy (63%)
In the week before the survey was completed, patients reported a range of additional symptoms highlighting the mental toll the condition takes. The symptoms required a median of 20 interventions for treatment and included:13
| Feeling unease (93%) | Fearfulness (82%) |
| Overwhelmed by worries (81%) | Feelings of helplessness (80%) |
| Anxiety (76%) | Depression (76%) |
| Hopelessness (72%) | Worthlessness (49%) |
“In this study,” the researchers explained, “individuals who reported PVS after COVID-19 vaccination had low health status, high symptom burden, and high psychosocial stress despite trying many treatments. There is a need for continued investigation to understand and treat this condition.”14
Even a 2021 study reported a series of patients who experienced new autoimmune conditions — or flare-ups of existing autoimmune disease — following mRNA COVID-19 shots,15 highlighting the importance of careful research into the ongoing health risks.
Will Long Vax Be Censored?
It’s hopeful that scientific on long vax is reaching medical journals and getting some media coverage.16 But Kory and Marik are concerned it could reach a similar fate as other COVID shot coverage during the pandemic.
“The concern is that our findings, Krumholz’s study, and any reports of adverse events from COVID-19 vaccination, will be subject to the same institutional censorship we saw throughout the pandemic. Suppressing this information risks creating an even bigger disaster,” they told The Hill,17 referring to a potential epidemic of autoimmune diseases that could occur as a result.
“America’s health agencies need to snap into action to help study this problem so we can better understand and treat these conditions. Unfortunately, there doesn’t seem to be much hope of this happening,” Kory and Marik wrote. “The National Institutes of Health is fixated on studying the effect of Paxlovid, an antiviral COVID treatment, to treat long COVID and long vax, despite it having no proven effect on autoimmune disease.”18
Further, Kory explains that while major medical centers and hospitals across the U.S. have opened long COVID clinics, the treatments they offer are largely ineffective, and they often gas-lit long vax patients who tried to get help:19
“[F]or most of 2022 into 2023, those centers consistently gas-lit the Long Vax patients who presented to those clinics. Gaslighting of medical injuries is the well-described inability for physicians to recognize or accept when their own treatments (i.e the mRNA vaccines) cause harm …
The stories my patients would tell me of the care they received included what I would describe as abuse or insults from the treating physicians when the patients tried to convince them that the vaccines were the cause. These stories still make my blood boil and have estranged many of my patients from ‘the system.’ I believe the gaslighting responses have lessened somewhat but I don’t really know how much.
What angered me even further is that the health agencies only directed funding at long COVID and the medical literature and media only referred to sufferers as having long COVID. The contribution of the gene therapy vaccines are consistently ignored.”
Is Long Vax Behind the Explosion of Disability Claims?
Kory believes that long vax, and to a lesser extent long COVID, are behind the explosion of disability claims that have occurred since COVID-19 shots rolled out.20
Data compiled by former BlackRock analyst and fund manager Edward Dowd revealed a sobering glimpse into the true carnage that occurred at the hands of the COVID-19 shot campaign,21 and its results are striking. It revealed the following estimated human and economic costs:22
Human cost:
- 26.6 million injuries
- 1.36 million disabilities
- 300,000 excess deaths
Economic cost:
- Total: $147.8 billion
- Injuries: $89.9 billion
- Disabilities: $52.2 billion
- Excess deaths: $5.6 billion
What’s more, this data is from the employed population, aged 16 to 64 — a typically healthy crowd. To put this into perspective, John Leake writes on Courageous Discourse, “Note that this death count in one year is 5.2 times the number of men killed in ten years of combat in Vietnam.”23
Help for Long Vax Symptoms
As long vax and its symptoms become increasingly recognized, it will hopefully lead to increased access to effective treatments. If you’re experiencing symptoms, it’s important to find a holistic health care practitioner who’s familiar with long vax and how to treat it. You can also access FLCCC’s I-RECOVER24 guide,25 which offers step-by-step instructions on how to treat reactions from COVID-19 injections.26
I also summarized strategies to optimize mitochondrial health if you’re suffering from long COVID or long vax, with a focus on boosting mitochondrial health. To allow your body to heal you’ll want to minimize EMF exposure as much as possible. Your diet also matters, as the cristae of the inner membrane of the mitochondria contains a fat called cardiolipin, the function of which is dependent on the type of fat you get from your diet.
The type of dietary fat that promotes healthy cardiolipin is omega-3 fat, and the type that destroys it is omega-6, especially linoleic acid (LA), which is highly susceptible to oxidation. So, to optimize your mitochondrial function, you want to avoid LA as much as possible and increase your intake of omega-3s.
Primary sources of LA include seed oils used in cooking, processed foods and restaurant foods made with seed oils, condiments, seeds and nuts, most olive oils and avocado oils (due to the high prevalence of adulteration with cheaper seed oils). Animal foods raised on grains, such as conventional chicken and pork, are also high in LA.
Another major culprit that destroys mitochondrial function is excess iron — and almost everyone has too much iron. You can learn more about the health risks of excess iron in my interview with Christy Sutton, D.C. The most effective way to lower your iron is to donate blood two to four times a year.
Copper is also important for energy metabolism, detoxification and mitochondrial function, and copper deficiency is common. Other strategies include sun exposure and near-infrared light therapy, NAD+ optimizers and methylene blue, which can be a valuable rescue remedy. By improving your mitochondrial function and restoring the energy supply to your cells, you’ll significantly increase your odds of reversing the problems caused by the jab or the virus.
- 1 U.S. CDC, MMWR February 15, 2024 / 73(6);135–136
- 2, 3, 4, 5, 19, 20 Pierre Kory’s Medical Musings March 8, 2024
- 6 TNR December 8, 2022
- 7 Science January 20, 2022
- 8, 9, 10 medRxiv May 17, 2022
- 11, 12, 13, 14 medRxiv November 10, 2023
- 15 Int Immunopharmacol. 2021 Oct:99:107970. doi: 10.1016/j.intimp.2021.107970. Epub 2021 Jul 10
- 16, 17, 18 The Hill March 6, 2024
- 21 Phinance Technologies, The Vaccine Damage Project March 2023
- 22 Zero Hedge March 28, 2023
- 23 Substack, Courageous Discourse March 29, 2023
- 24, 25 FLCCC Alliance, I-RECOVER
- 26 FLCCC Alliance, I-RECOVER, Post-Vaccine Treatment Guide
Canola Oil Proven to Destroy Your Body and Mind
Reproduced from original article:
https://articles.mercola.com/sites/articles/archive/2024/03/18/canola-oil-health-effects.aspx
The original Mercola article may not remain on the original site, but I will endeavor to keep it on this site as long as I deem it to be appropriate.
Analysis by Dr. Joseph Mercola March 18, 2024

STORY AT-A-GLANCE
- According to AARP, 93% of Americans are concerned with their brain health, but few understand how to protect it
- Research demonstrates canola oil led to significant declines in working memory and has a significant impact on weight management
- Canola oil is not healthy fat vital to your brain; it is manufactured from genetically engineered rapeseed plants altered to reduce levels of erucic acid toxic to humans and processed through several chemical baths before being bleached
- Healthier options include pastured, organic butter, virgin coconut oil, ghee (clarified butter) and lard for cooking and olive oil for non-cooking purposes
According to a study by AARP,1 93% of Americans are concerned with their brain health, but very few understood some of the natural strategies they could use to improve it. Contrary to popular belief, your brain function and cognitive performance do not have to decline with age. There are steps you can take that influence your memory, processing, executive functions and more.
Even if you are already in your “golden years,” simple changes may prompt brain health for the better. For instance, where once it was believed that neurons were only generated early in life, scientists now know that neurogenesis (generation of new neurons) continues into adulthood.2 Exactly what influences the rate of new neuron growth is still being explored, as are other factors that play a role in brain health.
Research, for instance, has uncovered damage canola oil consumption triggers in your brain and the effect this may have on your memory and learning ability.3 The study, published in the journal Nature, also found the consumption of canola oil increased weight gain.
Canola Oil Negatively Affects Brain Health and Weight Management
The study was led by researcher Dr. Domenico Praticò from Lewis Katz School of Medicine at Temple University in Philadelphia, Pennsylvania. Praticò commented to the Los Angeles Times that canola oil is perceived by many to be healthy — a widespread misconception:4
“Canola oil is appealing because it is less expensive than other vegetable oils, and it is advertised as being healthy. Very few studies, however, have examined that claim, especially in terms of the brain.”
Researchers used an animal model to evaluate the effect canola oil has on the brains of mice genetically engineered to develop Alzheimer’s disease.5 Canola oil developed a reputation of being healthy when doctors began warning people to reduce their saturated fat intake and consume vegetable oils instead. Canola has the lowest percentage of saturated fat of all commonly used vegetable oils and is relatively inexpensive, but is actually one of the worst oils for your health.
Canola oil is often used in homes and restaurants for baking, sautéing, frying and other forms of cooking, with consumers being deceived into believing it’s better for them than saturated fats. The mice were split into two groups; one group was fed the usual chow and the second group was fed chow with the human equivalent of 2 teaspoons of canola oil per day.
At the end of the experimental six months, researchers observed that the mice eating chow laced with canola oil were significantly heavier than the mice that did not eat canola oil. Additionally, the mice who had eaten canola oil demonstrated significant declines in working memory together with a decreased level of post-synaptic density protein-94, a marker of synaptic integrity. The researchers found canola oil had a negative effect on health and concluded:6
“Taken together, our findings do not support a beneficial effect of chronic canola oil consumption on two important aspects of AD [Alzheimer’s disease] pathophysiology which includes memory impairments as well as synaptic integrity.”
Your Brain Needs Healthy Fats
The same researchers used a similar model to evaluate the effects of olive oil on the brain function of mice.7 In that study,8,9 neither group was heavier than the other, and the mice fed chow enriched with extra-virgin olive oil performed significantly better on testing that evaluated the animals’ working memory, spatial memory and ability to learn.
The brain tissue of these mice, genetically engineered to develop Alzheimer’s disease as they age like the mice in the featured study, also revealed dramatic differences. The mice fed olive oil demonstrated preserved synaptic integrity and an increase in nerve cell autophagy, ultimately responsible for a reduction in amyloid plaques common in the brain of those with Alzheimer’s disease.10
Healthy fat is an essential component of the structure of your brain, which is composed of nearly 60% fat.11 It should come as no surprise that your brain needs quality fat to function optimally. Although your brain is a small part of your complete bodyweight, it uses 20% of your metabolic energy. Essential fatty acids are required but cannot be synthesized in your body, and so must come from dietary sources.
Most people get well over what is needed of omega-6 fats, which are found in most vegetable oils, and not nearly enough omega-3 fats. One omega-3 fat, DHA, has been linked with the growth of your retina and visual cortex during development,12 visual acuity and reduction in depression. Research has found those suffering from attention deficit hyperactivity disorder (ADHD) have lower levels of DHA, and DHA may play a role in neuroprotection.
Unlike the highly damaged fats in vegetable oil, saturated fat is the optimal “clean” fuel for your brain and is one of the main components of brain cells. As such, it’s excellent for brain health, with one study demonstrating that those who ate more saturated fat reduced their risk of developing dementia while those who favored carbohydrates had a significantly increased risk.13
To maintain optimal brain function, you need high-quality, undamaged omega-3s and omega-6 along with antioxidants to protect them from oxidation — not processed vegetable oils like canola oil. In summary, processed vegetable oils are bad for your brain health for a number of reasons, including the following:
- They are loaded with damaged omega-6 fatty acids without protective antioxidants
- They strip your liver of glutathione, which produces antioxidant enzymes, which further lowers your antioxidant defenses
- Most vegetable oils are made with genetically engineered (GE) crops designed to resist herbicides like glyphosate. As such, they may be more contaminated with glyphosate than non-GE crops, and glyphosate has been shown to disrupt the tight junctions in your gut and increase penetration of foreign invaders, especially heated proteins, which can cause allergies

Save This Article for Later – Get the PDF Now
Vilification of Healthy Fats Has Contributed to Rising Rates of Disease
Defaming healthy fats over the past decades has contributed to a rising rate of disease. Although healthy fats are used as fuel and leave you feeling full, many turned to eating carbohydrates when fats were discouraged. Carbs are metabolized and burned quickly, using insulin to usher blood glucose into the cell.
However, carbs trigger insulin resistance over time and increase the potential for crashing blood sugar levels two to three hours after a meal, leaving you hungry once again and increasing your food intake. This one mechanism increases your risk for obesity, which in turn increases your potential risk for insulin resistance, Type 2 diabetes, cardiovascular disease and stroke.
In a time when healthy saturated fats and dietary cholesterol were publicly slandered, Canada developed an alternative oil that met with the approval of the American Heart Association (AHA) — canola oil.14 Now sitting in the first position of recommended oils for healthy cooking on the AHA website, author Praticò had this to say about the results of his canola oil study:15
“Amyloid-beta 1-40 neutralizes the actions of amyloid 1-42, which means that a decrease in 1-40, like the one observed in our study, leaves 1-42 unchecked. In our model, this change in ratio resulted in considerable neuronal damage, decreased neural contacts, and memory impairment.”
In other words, consuming canola oil may increase your risk of developing Alzheimer’s disease, as the oil decreases the production of a protein that protects your brain against neuronal damage and cognitive impairment.
Toxicity of Canola Oil May Result From the Seed, Source or Processing
This short video shows you the conditions under which canola oil is manufactured and produced, including the deplorable number of chemicals and bleaches added to the product to achieve the clear liquid you see on your grocery store shelves. Just the way the oil is processed should be enough to encourage you to steer clear of consuming the product. But the risk associated with canola oil doesn’t stop with processing.
The canola plant was developed from rapeseed plants by Agriculture and Agri-Food Canada and the University of Manitoba using plant breeding techniques. In fact, the Canola Council of Canada calls the development, “Canada’s greatest agricultural success story.”16 Rapeseed oil was originally used as a motor lubricant during World War II.17 Once the war ended, demand plummeted and Canada began an intensive program to make the product edible.
Before it could be ingested the erucic acid and glucosinolates had to be bred out of the plant, as they are dangerous to human health.18 By the late 1970s, both chemicals were reduced to lower levels, and the plant was officially accepted as consumable. In the 1980s, research focused on shelf stability of the oil, animal diets and gaining a wider consumer acceptance.
By 2012, nearly all low-erucic acid rapeseed plants were genetically engineered to increase yield. Today, what began as a motor lubricant is now one of Canada’s most profitable crops.
The featured study evaluated the effect of canola oil on brain function without identifying which characteristic of the product triggers the problems. However, as most canola oil is produced from GE seeds, using plants originally unfit for human consumption and taken through a process that injects multiple chemicals and bleaches, it isn’t surprising the study was so conclusive.
Genetic Engineering Raises Health Risk With Each GE Food Consumed
This documentary details what happens when we use GE foods. Scientists are only beginning to uncover the long-term effects of splicing the genes of one living creature into another or developing a plant immune to the effects of herbicides.
However, some companies are not convinced by independently funded research and have relied on information from organizations such as the American Medical Association (AMA) and World Health Organization (WHO), which claim there is no credible evidence that GE foods are unsafe. However, even WHO admits:19
“Different GM [genetically modified] organisms include different genes inserted in different ways. This means that individual GM foods and their safety should be assessed on a case-by-case basis and that it is not possible to make general statements on the safety of all GM foods.”
In 2015, the European Commission decided it was in the best interest of their citizens to say “no” to genetically modified organisms (GMOs) within their borders, and all 28 countries required labeling of foods containing GMO products.20 This is in stark contrast to the U.S., where most canola grown is GE21 and products created from it not labeled as such.
Healthy Cooking Options
Cooking with nearly all vegetable oils is problematic as they don’t tolerate high heat. Healthier options for cooking include pastured, organic butter, virgin coconut oil, ghee (clarified butter) and lard. Olive oil and sesame oil add wonderful flavor and healthy fats to your foods, but they have very low smoke points and should be used unheated in salad dressings or drizzled over meats or vegetables for flavor.
Boosting Brain Health Naturally
It is never too late to support your neurological health. Remember, even small changes you make each day reap big rewards over time. Seek to change your habits consistently and persistently to support your memory, cognitive function and ultimately your enjoyment of everyday life. Here are several strategies you may use to improve your brain health:
| Vitamin D — There are strong links between low levels of vitamin D in Alzheimer’s patients and poor outcome on cognitive testing. Optimal vitamin D levels may protect brain cells by increasing the effectiveness of the glial cells in restoring damaged neurons. Additionally, vitamin D has anti-inflammatory properties. |
| Carotenoids — These antioxidant compounds are found most often in orange colored vegetables, such as sweet potatoes and carrots. Some carotenoids, such as lutein and zeaxanthin, are found in dark green vegetables, namely kale and spinach (as well as egg yolks). Lutein and zeaxanthin are best known for the role they play in vision health, but accumulating evidence suggests they play a role in cognitive health as well by enhancing neural efficiency.22 |
| Probiotics — You are likely familiar with the importance of probiotics for your gut health but may not know of the role they play in your cognitive health. Certain beneficial bacterial strains, such as those found in fermented foods, have a positive effect on your brain function.
In a study by the University of California Los Angeles, scientists found women who regularly consumed beneficial bacteria via yogurt experienced changes in multiple areas of their brain, including those related to sensory processing, cognition and emotion.23 |
| Exercise — Physical activity produces biochemical changes that strengthen and renew not only your body but also your brain — particularly areas associated with memory and learning. |
| Diet — Reducing overall calorie and carbohydrate consumption, while increasing healthy fats, has a powerful effect on your brain health. Beneficial health-promoting sources of healthy fats that your body — and your brain in particular — needs for optimal function include organic grass fed raw butter, olives, organic virgin olive oil and coconut oil, nuts like pecans and macadamia, free-range eggs, wild Alaskan salmon and avocado, for example.
Increasing your omega-3 fat intake and reducing consumption of damaged omega-6 fats (i.e., processed vegetable oils) in order to balance your omega-3-to-omega-6 ratio also has a significant benefit for your brain. |
| Sleep — Sleep not only is essential for regenerating your physical body, but imperative for reaching new mental insights and being able to see new creative solutions to old problems. Sleep removes the blinders and helps “reset” your brain to look at problems from a different perspective.
Research from Harvard indicates that people are 33% more likely to infer connections among distantly related ideas after sleeping,24 but few realize that their performance has actually improved. Sleep is also known to enhance your memories and help you “practice” and improve your performance of challenging skills. In fact, a single night of sleeping only four to six hours can impact your ability to think clearly the next day. |
- 1 AARP, January 20, 2015
- 2 Brain Aging: Models, Methods and Mechanisms
- 3, 6 Nature, 2017;7(17134)
- 4, 5 Los Angeles Times, December 11, 2017
- 7 Science Daily, June 21, 2017
- 8 Ann Clin Transl Neurol. 2017 Jun 21;4(8):564-574
- 9, 10 EurekAlert! June 21, 2017
- 11, 12 ACTA Neurology Taiwan, 2009; 18:231
- 13 Journal of Alzheimer’s Disease, 2012;32(2): 329
- 14 American Heart Association, Healthy Cooking Oils
- 15 Forbes, December 11, 2017
- 16 Canola Council of Canada
- 17 Small Footprint Family, The Inconvenient Truth About Canola Oil
- 18 Canola History, Good as Gold
- 19 World Health Organization, Food, genetically modified
- 20 Library of Congress, Restrictions on genetically modified organisms
- 21 Agricultural Marketing Resource Center, Canola Profile February 2022
- 22 Journal of International Neuropsychological Society, 2016; 23(1):11
- 23 Gastroenterology. 2013 Jun;144(7):1394-1401.e4
- 24 New York Times September 27, 2008
Latest Additions to Long COVID Recovery Protocol
Reproduced from original article:
https://articles.mercola.com/sites/articles/archive/2024/02/24/long-covid-recovery-protocol.aspx
The original Mercola article may not remain on the original site, but I will endeavor to keep it on this site as long as I deem it to be appropriate.
Analysis by Dr. Joseph Mercola February 24, 2024
STORY AT-A-GLANCE
- The Front Line COVID-19 Critical Care Alliance has updated its treatment protocols for long COVID and post-jab injuries, adding time-restricted eating (TRE) and photobiomodulation (PBM), using either the sun or near-infrared sauna
- The primary benefit of TRE for these conditions is its ability to optimize your mitochondrial function, which is key for recovery from any illness or disease. As a general rule, I recommend compressing your eating window to between six and eight hours, and fasting for the remaining 16 to 18 hours each day
- Near-infrared light triggers production of melatonin in your mitochondria. Melatonin is one of the most important antioxidant molecules in your body. Aside from having direct antioxidant effects, it also stimulates the synthesis of glutathione and other important antioxidants
- Fifty-three percent of sunlight is near-infrared. Sauna Space also makes near-infrared sauna bulbs that mimic the sun, providing 39% near-infrared light, but no UV
- You can further optimize your mitochondria by combining PBM with methylene blue. This combination has been shown to provide neuroprotective benefits. It can also address the chronic fatigue that is so common in long COVID and post-jab injuries
The video above features the Front Line COVID-19 Critical Care Alliance’s (FLCCC) weekly update for October 26, 2022, in which I reviewed the benefits of two of the latest additions to the FLCCC’s long COVID recovery protocol,1 and their post-jab recovery protocol:2 time-restricted eating (TRE) and photobiomodulation using either the sun or a near-infrared sauna. Leading the discussion are FLCCC cofounders Dr. Paul Marik and Dr. Pierre Kory.
Time-Restricted Eating (TRE)
The vast majority of people eat across 12 hours or more, which is a recipe for metabolic disaster. Health statistics bear this out. In July 2022, the Journal of the American College of Cardiology3 posted an update on the metabolic fitness or flexibility of the American population.
Metabolic fitness includes things like blood glucose and blood sugar, blood pressure and weight, and metabolic flexibility refers to your body’s ability to seamlessly transition between burning fat and carbohydrates as your primary fuel.
In 2016, 12.2% of Americans were considered metabolically fit.4 Two years later, in 2018, only 6.8% of U.S. adults had optimal cardiometabolic health.5 That was four years ago, so today, that ratio is probably even lower.
I believe at least 95% of Americans are by now metabolically unhealthy, which means some 19 out of 20 people would benefit from TRE, as it’s one of the easiest yet most powerful interventions for reducing insulin resistance, restoring metabolic flexibility and losing excess body fat.
As it pertains to long COVID and post-jab recovery, the primary benefit of TRE is its ability to optimize your mitochondrial function, which is key for recovery from any illness or disease.
As a general rule, I recommend compressing your eating window to between six and eight hours, and fasting for the remaining 16 to 18 hours each day. The timing of that eating window is important though.
You want to avoid eating first thing in the morning (wait at least two or three hours) and you want to avoid eating right before bed. Ideally, have your last meal at least three hours or more before bedtime. So, to give you an example, you could eat all your meals between 10 a.m. and 6 p.m., or 11 a.m. and 5 p.m.
Near-Infrared Exposure and Melatonin
Another important mitochondrial tool is strategic use of near infrared light and its impact on melatonin, which is one of the most important antioxidant molecules in your body. Aside from having direct antioxidant effects, it also stimulates the synthesis of glutathione and other important antioxidants like superoxide dismutase and catalase.
While commonly thought of as something produced only in the pineal gland of your brain, which is produced in response to darkness, it only accounts for 5% of the melatonin in your body. A couple of years ago, Dr. Russel Reiter published a groundbreaking paper explaining that the vast majority, 95%, is actually made within the mitochondria inside your cells,6 where it is produced in response to near-infrared light, which could be from the sun or near-infrared sauna bulbs.
Considering melatonin combats oxidative damage, it makes sense that most of it is made in your mitochondria, because that’s precisely where a majority of the oxidative damage occurs — in the mitochondrial electron transport chain. So, it’s a truly phenomenal system. The key that makes this system work, however, is exposure to near-infrared light. To dive deeper into this topic, see my interview with Reiter.
This is one of the reasons why exposing as much bare skin as possible to the sun for an hour a day is my No. 1 recommendation to optimize your health. And it’s free. As you can see in the graph below, 52% of the sun’s rays are near-infrared.
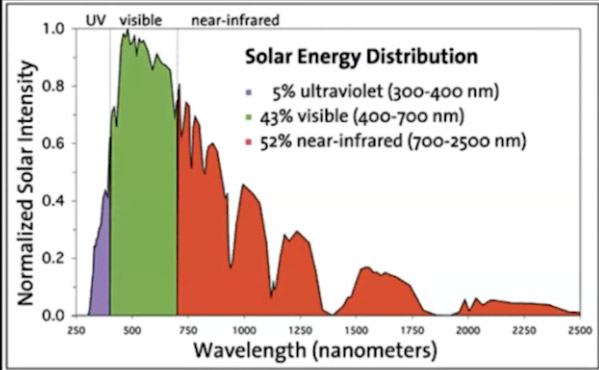

Download this Article Before it Disappears
Concerning Skin Cancer
As noted by Marik, many shy away from sun exposure as a source of UV and near IR for fear of skin cancer. This is yet another example of medical propaganda. The fact is the sun is a nutrient that will actually decrease your risk of both skin cancer and internal cancers, provided you avoid sun burn.
Another little-known fact is that the fats in your diet can, to a significant degree, dictate how predisposed you are to burning and sun-related skin damage. The key is to limit omega-6 fats in your diet. That means avoiding processed foods, foods cooked in seed oils, and animal foods raised on seed oils and/or grains, such as chicken and pork.
Omega-6 seed oils are primarily linoleic acid (LA), a polyunsaturated fat that is highly susceptible to oxidative damage when exposed to a variety of stressors. What’s more LA can remain embedded in your cell membranes and tissues for up to seven years, all the while wreaking havoc and causing damage through oxidative stress.
As it pertains to sun exposure, the LA embedded in your cell membranes gets activated by the exposure to the sun, which contributes to skin damage. Once you drastically reduce or eliminate LA from your diet, your risk of sunburn will be dramatically reduced over time, as will your risk of skin cancer.
General Benefits of Photobiomodulation (PBM)
Light in the red and infrared range has several important health benefits, including:
| Increasing mitochondrial ATP production | Increasing heat shock proteins, which help proteins maintain their three-dimensional structure and refold misfolded proteins |
| Activating cell stress responses | Increasing autophagy |
| Reducing inflammation | Speeding up wound healing |
Near-infrared light specifically, which is invisible to the naked eye, can penetrate 5 to 7 inches into your body, into your subcutaneous tissue, muscle tissue, bone and even interior tissues as you can see by the graphic below. This is in stark contrast to far IR that most saunas use, which penetrates less than half an inch.

This is what makes near-infrared saunas so useful, as you can boost melatonin production throughout your entire body, including your organs, thereby detoxing and healing them. In comparison, far-infrared penetrates only 1 to 2 millimeters, yet far-infrared is, unfortunately, what most commercially available electrical saunas use.
General Benefits of Sauna Therapy
Research has demonstrated sauna use can:
| Improve cardiovascular fitness and lower your risk of death from cardiovascular disease, stroke and heart attack |
| Lower your blood pressure |
| Lower your risk of dementia |
| Improve your mood and mental health, and reduce symptoms of depression, in part by sensitizing opioid receptors |
| Strengthen your immune function |
| Reduce all-cause mortality |
| Improve athletic endurance |
| Reduce inflammation by lowering c-reactive protein, and increasing IL-10 and IL-6 (aka, myokine), and activating Nrf2 |
| Activate and replenish stem cells |
| Improve fasting glucose and insulin sensitivity |
| Reduce the stress hormone cortisol7 |
All of these benefits occur in a dose-dependent manner, so the more frequent your sauna use, the more robust your benefits will be. For example, using the sauna two to three times a week has been shown to reduce your risk of cardiac death by about 22% compared to once-a-week use, whereas those who use it seven times a week lower their risk by 63%.
Similarly, those who use it four to seven times a week have a 40% lower all-cause mortality risk than those who use it only once a week. To learn more about these and other health benefits of sauna therapy, see “The Stunning Health Benefits of Sauna Therapy.”
Different Saunas Provide Different Sets of Benefits
Many of the benefits listed above are related to the heat exposure alone, and for heat, it doesn’t much matter what type of sauna you use: a traditional thermal Finnish sauna, a far-infrared sauna or a near-infrared one. Although one needs to be careful as many far IR saunas simply do not get hot enough to generate heat shock proteins and detox.
Near-infrared saunas have benefits that you simply cannot get with the others. Below is a simple chart showing the differences in benefits between the three primary types of saunas available in the U.S.

As you can see, all will provide detoxification to some degree (although the detox provided by far-infrared is questionable, seeing how it barely penetrates your tissue. Far-infrared saunas also oftentimes cannot get hot enough for efficient detox, which requires you to sweat profusely). Detoxification is something just about every person needs, as we’re surrounded by toxins and take them in with both food and water.
Unstructured proteins tend to aggregate, and these aggregates can then form plaques in your vascular system or brain, contributing to neurodegenerative diseases and cardiovascular problems. Heat shock proteins serve a really crucial role in keeping these kinds of problems at bay.
All three will also generate heat shock proteins to some degree. As mentioned earlier, heat shock proteins are important because they refold misfolded proteins and all of us have misfolded proteins.
Unstructured proteins tend to aggregate, and these aggregates can then form plaques in your vascular system or brain, contributing to neurodegenerative diseases and cardiovascular problems, so heat shock proteins serve a really crucial role in keeping these kinds of problems at bay.
Again, there’s a question mark by far-infrared, as many far-infrared saunas can’t get hot enough. Near-infrared saunas also are nowhere near as hot as the Finnish-style sauna, but they don’t need to be, due to the extreme penetration. You’ll sweat profusely and activate heat shock proteins even though the air temperature is lower than a Finnish thermal sauna.
You can determine if your sauna is hot enough for you by measuring your temperature with an oral thermometer. It should be around 101 to 103 degrees Fahrenheit as you finish your sauna. You could also weigh yourself before and after the sauna and you should lose between 2 and 4 pounds of water (sweat). This would be one pint to one quart of water.
Next on the list, melatonin production. This can only be achieved in a near-infrared sauna, as melatonin is not produced in response to mere heat or light in the far-infrared range.
The Importance of an EMF-Free Sauna
Lastly, there’s the issue of adverse health effects of electromagnetic fields (EMF). I published a book about this in early 2020, called “EMF*D.” Virtually no far-infrared saunas on the market are truly EMF-free, even when advertised as such. The reason for this is because EMFs include both electric and magnetic fields, and most saunas address only one of these.
If you’re using a wood-burning Finnish sauna, it will of course be EMF-free, but almost no one has that in the U.S. Most Finnish-style saunas sold here use electrical heaters and emit electrical fields. When you’re detoxing, you want to be in a parasympathetic environment. When you’re exposed to EMFs, it activates your sympathetic nervous system, which impairs your ability to detox properly.
The near-infrared Sauna Space sauna that I use and recommend has no EMFs. And, again, while traditional and some FIR saunas can provide outstanding benefits in detox and heat shock protein generation, neither of them provide the light wavelengths to generate PBM benefits.
What Make Sauna Space’s Bulbs so Unique
Sauna Space uses incandescent heat lamps (shown in the photo further below) that produce the majority of the heat as mid-infrared, plus a significant percentage of near- and mid-infrared frequencies that provide PBM benefits. The spectral distribution of these bulbs is shown in the following graph.
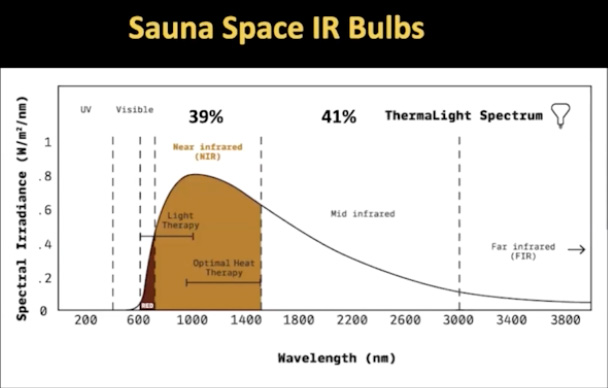
As mentioned, 53% of sunlight is near-infrared, and the Sauna Space bulbs mimic sunlight with 39% of the light being in the near-infrared range. (They do not have any UV light, however, so you will not make vitamin D. The bulbs only mimic sunlight in terms of their infrared distribution.) This is vastly superior to the average red heat lamp (graph below), in which only 14% is near-infrared.
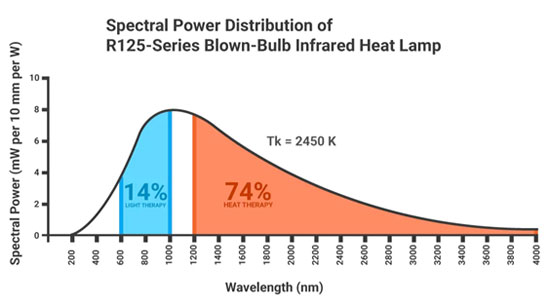
In “Near-Infrared Sauna Therapy — A Key Biohack for Health,” I provide instructions for how you can create your own near-infrared sauna using the Sauna Space near-infrared bulbs.
Sauna Space is the only company that I know of that makes these kinds of bulbs, so they’ve really cornered the market, at least for now. Using these, you’ll be able to make the absolute best, most effective sauna there is, as you’re getting both the standard sauna benefits and the PBM benefits, and none of the EMF hazards.

Optimizing Photobiomodulation With Methylene Blue
If you want to further optimize your mitochondria, you can combine PBM (the near-infrared light) with methylene blue. A 2020 paper8 in Translational Neurodegeneration reviews the benefits of this combination, specifically as it refers to neuroprotection. I believe this combination can also be very valuable in the treatment of long COVID and in post-jab recovery, many symptoms of which are neurological in character.
In 1890, the German physician Dr. Paul Ehrlich published a study showing methylene blue could effectively treat malaria. Interestingly, many of the most useful drugs for COVID are antimalarial and antiparasitic drugs such as hydroxychloroquine. Well, methylene blue is the parent molecule to chloroquine.
Methylene blue can be particularly useful for addressing the fatigue that is so common in long COVID. You can learn more in “The Surprising Health Benefits of Methylene Blue,” in which I interview Francisco Gonzalez-Lima, Ph.D., who has spent many years studying this drug.
In closing, you can find the latest, updated protocols for long COVID9 and post-jab injuries10 on the FLCCC’s website. These protocols are continually updated as the team learns more.
- 1, 9 FLCCC Alliance, I-RECOVER Long COVID Treatment
- 2, 10 FLCCC Alliance, I-RECOVER Post-Vaccine Treatment Protocol
- 3 Journal of the American College of Cardiology July 2022; 80(2): 138-151
- 4, 5 Metab Syndr Relat Disord February 2019; 17(1): 46-52
- 6 Physiology February 5, 2020
- 7 YouTube The Science & Health Benefits of Deliberate Heat Exposure | Huberman Lab Podcast #69
- 8 Translational Neurodegeneration 2020; 9: 19
Liposomal Carnosine Is Essential for Detoxing Linoleic Acid
Reproduced from original article:
https://articles.mercola.com/sites/articles/archive/2024/02/05/liposomal-carnosine.aspx
The original Mercola article may not remain on the original site, but I will endeavor to keep it on this site as long as I deem it to be appropriate.
Analysis by Dr. Joseph Mercola February 05, 2024

STORY AT-A-GLANCE
- Carnosine is a dipeptide found in meat. The highest concentrations of carnosine are found in your muscles, brain, central nervous system and gastrointestinal tract
- If you’re a vegetarian or vegan, you will have lower levels of carnosine in your muscles. This is one reason why many strict vegans who do not properly compensate for this tend to have trouble building muscle
- Carnosine binds to advanced lipoxidation endproducts (ALEs) that form from oxidized seed oils in your diet, making it a crucial aid in the detoxification of linoleic acid (LA)
- Thanks to its ability to scavenge 4-hydroxynonenal (4HNE), carnosine is also protective against obesity, diabetes, cardiovascular disease and Alzheimer’s disease, just to name a few
- The best way to optimize your carnosine level is to eat organic grass fed beef. When it comes to carnosine supplements, your best bet is liposomal versions as they have the highest bioavailability
Carnosine is a dipeptide found in meat. It’s not found in any plant foods. Dipeptide means it’s made up of two amino acids, in this case beta-alanine and histidine. The highest concentrations of carnosine are found in your muscles, brain, central nervous system1 and gastrointestinal tract,2 which gives you an indication of its potential importance.
Unfortunately, it’s also one of the top 10 most common nutrient deficiencies, especially among vegans. If you’re a vegetarian or vegan, you will have lower levels of carnosine in your muscles. This is one reason why many strict vegans who do not properly compensate for this tend to have trouble building muscle.
Carnosine also binds to advanced lipoxidation endproducts (ALEs) that form from oxidized seed oils in your diet, making it a crucial aid in the detoxification of linoleic acid (LA).
Carnosine’s Physiological Roles
Carnosine has several physiological roles and benefits. For example, it:3
| Provides athletic benefits — Approximately 99% of carnosine is found in muscle tissue where it facilitates lactic acid detoxification, improves muscle contraction and muscle relaxation and enhances endurance |
| Alleviates diabetic nephropathy by protecting podocyte and mesangial cells4 |
| Modulates energy metabolism in macrophages and microglia by restoring and/or enhancing the basal conditions |
| Has antioxidant properties and scavenges reactive oxygen species (ROS) and aldehydes created by peroxidation of fatty acid cell membranes during oxidative stress5 |
|
Regulates the activity of stem cells |
| Modulates glucose metabolism |
| Enhances the degradation and/or scavenging of nitric oxide (NO) |
| Promotes wound healing |
| Opposes glycation6 |
| Slows down the aging process by prolonging the life of cells and preserving cellular homeostasis7 |
| Regulates osmotic pressure |
| Modulates glutamate production and transport |
| Modulates brain metabolism |
| Chelates heavy metals8 |
| Acts as a pH buffer9 |
| Acts as a neurotransmitter |
| Protects olfactory receptor neurons in the elderly |
Beef, Liposomal Carnosine and Precursors Are the Best Sources
Interestingly, a June 2023 paper10 in the medical journal Pharmaceuticals reviewed the science behind carnosine with the aim of developing new delivery systems for carnosine-based drugs. As noted in this paper:
“Because of its well-demonstrated multimodal pharmacodynamic profile, which includes anti-aggregant, antioxidant, and anti-inflammatory activities, as well as its ability to modulate the energy metabolism status in immune cells, this dipeptide has been investigated in numerous experimental models of diseases, including Alzheimer’s disease, and at a clinical level.
The main limit for the therapeutic use of carnosine is related to its rapid hydrolysis … [This is the] reason why the development of new strategies, including the chemical modification of carnosine or its vehiculation into innovative drug delivery systems (DDS), aiming at increasing its bioavailability and/or at facilitating the site-specific transport to different tissues, is of utmost importance.”
Delivery systems currently in use or in development include intraperitoneal injections, intranasal sprays and oral administration of various nanoformulations. But while the drug industry is keen on figuring out how to profit from carnosine by making it into a drug, you certainly don’t need a drug to get these benefits.
Simply eating organic grass fed beef is one of the most efficient ways to raise your carnosine level.11 This is one of many reasons why cultured beef is not a viable substitute for real beef. Not only does fake beef lack carnosine but also B vitamins, retinol, long-chain omega-3 fatty acids, taurine, creatine and bioavailable forms of iron and zinc.12
Most carnosine supplements aren’t very effective either because the carnosine is rapidly broken down into its constituent amino acids by certain enzymes. Your body then reformulates those amino acids back to carnosine in your muscles.
An exception to this is liposomal carnosine, which appears to work quite well. Another alternative is to supplement with beta-alanine, which is the rate limiting amino acid in the formation of carnosine. According to a 2021 paper,13 daily intake of beta-alanine can raise the carnosine content of skeletal muscle by as much as 80%.

Download this Article Before it Disappears
Carnosine Protects Against LA-Induced Oxidative Stress
One benefit not expounded upon in the Pharmaceuticals paper is carnosine’s ability to reduce LA-induced oxidative stress. While your body will slowly eliminate stored LA over time, provided you reduce your intake, carnosine can help reduce the oxidative damage caused by LA while your body is cleaning itself out. I take liposomal carnosine every day before meals to help detoxify LA.
The omega-6 fat LA is highly susceptible to oxidation, and as the fat oxidizes it breaks down into harmful sub-components such as ALEs and oxidized LA metabolites (OXLAMs). These ALEs and OXLAMs are what cause most of the damage.
Carnosine binds to ALEs like a magnet and acts as a sacrificial sink. It’s basically a substitute target for these profoundly damaging molecules. In this way, carnosine allows your body to excrete the ALEs from your body before they damage your mitochondria, DNA or proteins. (Another molecule that protects against LA-induced damage is carbon dioxide). The illustration below shows how carnosine works in this regard.
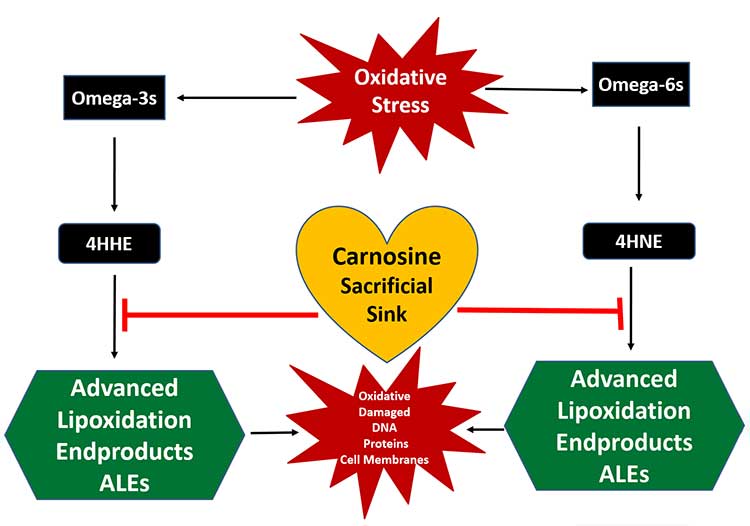
Carnosine May Be Protective Against a Wide Range of Diseases
A more detailed explanation of how carnosine protects against reactive oxygen species (ROS) and how that helps protect against oxidative stress-related pathologies is given in a 2021 paper in the journal Antioxidants:14
“A study that examined the effect of carnosine on oxidative stress in human kidney tubular epithelial (HK-2) cells indicated that carnosine decreased NADPH oxidase (NOX) 4 expression and increased total superoxide dismutase (T-SOD) activity, thus reducing the production of intracellular ROS, relieving the oxidative stress of cells, and ultimately inhibiting the mitochondrial pathway of apoptosis.
Ability of carnosine to protect against pathologies characterized by oxidative stress has been shown in a number of conditions … Carnosine changes the reactivity of superoxide anion by forming a charge-transfer complex with the superoxide radical and also by reducing the efficiency of hydroxyl radicals, creating a compound less reactive than the hydroxyl radical.
One of the mechanisms to protect organisms from oxidative stress is the chelation of transition metals, preventing them from participating in deleterious processes involving ROS … Interestingly, when comparing metals involved in free radical generation, carnosine was found to have a greater antioxidant activity coupled with copper than iron …
At physiological concentrations, carnosine directly reacts with superoxide anion similar to ascorbic acid. In physiological conditions, carnosine was found to reduce oxidative damage and to improve antioxidant activity of different antioxidative enzymes …
Experiments on aged rats showed that therapy with 250 mg/kg/carnosine per day significantly decreased oxidative stress and increased activity of antioxidative enzymes … In similar model of aged rats, carnosine increased liver vitamin E, which further demonstrates its importance in defending the organism from free radicals.
Rising data indicate that carnosine acts as a scavenger of reactive and cytotoxic carbonyl species including 4-hydroxynonenal (HNE). HNE is an aldehyde generated endogenously by lipid peroxidation of unsaturated fatty acids that act as ‘toxic second messengers,’ extending the harmful potential of free radicals.
HNE is considered an important biomarker of oxidative stress and accumulating data indicate that it may modulate signaling pathways of cell proliferation, apoptosis, and inflammation.”
How Carnosine Protects Against Alzheimer’s
As noted in the Pharmaceuticals paper,15 one of the pathologies that carnosine is protective against is Alzheimer’s disease. In my November 2021 interview with Tucker Goodrich, he explained the role of HNE, specifically, in Alzheimer’s, and why it’s so important to get rid of it.
“In heart failure, Alzheimer’s, and AMD [age-related macular degeneration], one of the things they see is an inability of the cell to produce enough energy. The mitochondria are getting damaged. HNE does that damage. It damages 24% of the proteins in the cell, primarily around energy production.
One of the ways your cells produce energy is they basically ferment glucose into pyruvate outside of the mitochondria. This is a perfectly normal part of metabolism and they produce something called pyruvate. A molecule called pyruvate dehydrogenase takes pyruvate into the mitochondria and converts it to acetyl-CoA so the mitochondria can burn it very efficiently for fuel.
Well, one of the things HNE does is it breaks pyruvate dehydrogenase, and they see this in Alzheimer’s where their cells are no longer able to produce enough energy. This is why your cells are dying in Alzheimer’s.
The beta amyloid plaques in Alzheimer’s disease are induced by HNE. There’s a great model that came out of Harvard a couple of years ago showing that.
Even the critical, the most important part of the mitochondria, complex 5, — ADP synthase — which is what takes all the energy coming from your mitochondria and turns it into ATP, which is what fuels the rest of your body — is damaged by HNE. This is a huge issue. There’s no more fundamental problem in aging and health than protein damage.”
Carnosine is the most effective scavenger of HNE, so optimizing your level can go a long way toward protecting against the HNE-induced damage that promotes Alzheimer’s.
Carnosine — A Promising Therapeutic for Obesity-Related Conditions
Elevated HNE has also been found in obese and diabetic patients,16 so there’s reason to suspect carnosine can be important in the treatment of these conditions as well. Another disease where elevated HNE plays a role is atherosclerosis. As noted in the 2021 Antioxidants paper:17
“… emerging studies have indicated that these reactive aldehydes are more than simply markers of oxidative stress.
Rather, it is suggested that these reactive species may play a significant pathogenic role in obesity-associated disorders such as insulin resistance and a carnosine analog alleviates the production or enhances the removal of reactive carbonyl species, providing promising new therapeutic compounds for cardiovascular and metabolic diseases related to obesity.”
Take Control of Your Health by Lowering Your LA Intake
As detailed in several previous articles, the evidence strongly suggests excessive LA is driving most if not all modern diseases, including heart disease and cancer. Fortunately, the solution is simple. Just lower your LA intake.
The easiest way to do this is to use an online nutritional calculator such as Cronometer to calculate your daily intake. Cronometer will tell you how much omega-6 you’re getting from your food down to the 10th of a gram, and you can assume 90% of that is LA. Anything over 10 grams is likely to cause problems. I keep my intake below 5 grams a day.
Since there’s no downside to limiting your LA, you’ll want to keep it as low as possible, which you do by avoiding high-LA foods. Keep in mind you’ll never be able to get to zero, and you wouldn’t want to do that either. You do need some LA, but since it’s found in most foods, and since you need only small amounts, there’s really no way to end up with a deficiency.
- 1, 3, 10, 15 Pharmaceuticals June 2023; 16(6): 778
- 2, 4, 5, 6, 7, 8, 9, 13, 14, 16, 17 Antioxidants July 2021; 10(7): 1037
- 11 Science Direct, Carnosine; Nutritional Supplements and Metabolic Syndrome
- 12 Animal Frontiers April 15, 2023
What’s the Best Predictor of Heart Disease?
Reproduced from original article:
https://articles.mercola.com/sites/articles/archive/2024/01/18/predictors-atherosclerosis.aspx
The original Mercola article may not remain on the original site, but I will endeavor to keep it on this site as long as I deem it to be appropriate.
Analysis by Dr. Joseph Mercola January 18, 2024
STORY AT-A-GLANCE
- High total cholesterol and/or elevated low-density lipoprotein (LDL) cholesterol do not cause atherosclerosis
- Low levels of high-density lipoprotein (HDL) cholesterol are associated with both atherosclerosis and insulin resistance, and insulin resistance appears to be the foundational cause of heart disease. As such, the fasting insulin test is one of the best predictors of atherosclerosis
- Insulin resistance is primarily driven by excessive consumption of the omega-6 fat linoleic acid (LA). High LA intake is also associated with elevated levels of oxidized LDL — found in atherosclerosis plaque — further confirming this link
- One theory is that oxidized LDL protects your body from oxidative damage by sacrificing itself. If true, it may be beneficial to have higher, rather than lower, LDL levels
- The apoB test can also be helpful in assessing your atherosclerosis risk. As mentioned above, apoB is the primary carrier for LDL, and research over the past decade shows it’s an accurate predictor of cardiovascular risk when apoB is high and LDL is normal
Is high total cholesterol and/or elevated low-density lipoprotein (LDL) cholesterol indicative of elevated heart disease risk? According to Dr. Paul Saladino, the answer is no. With regard to total cholesterol, as far back as 1977, with the publication of the Framingham Study,1 no correlation between heart disease and total cholesterol could be found.
Low levels of high-density lipoprotein (HDL) cholesterol was associated with coronary heart disease, but not high LDLs or total cholesterol. However, as noted by Saladino, low HDL is also associated with insulin resistance, and he believes this is part of the confusion.
Saladino suspects that what has been blamed on LDL (atherosclerosis) is due to insulin resistance, i.e., metabolic dysfunction. Insulin resistance/metabolic dysfunction, in turn, is primarily driven by excessive consumption of the omega-6 fat linoleic acid (LA).
High LA intake also raises your levels of oxidized LDL, which are what you find in atherosclerosis plaque. In the video above, Saladino and Dr. Nadir Ali specifically discuss the role of oxidized LDL, and why it is not a direct cause of atherosclerosis, as commonly thought.
Summary of Available LDL Tests
But before I summarize Saladino’s and Ali’s discussion, let’s take a look at the available LDL-related tests, as there’s more to LDLs than the total amount.
- A regular LDL cholesterol blood test (LDL-C), which measures the total amount of LDL cholesterol in your blood
- A nuclear magnetic resonance lipoprofile (NMR lipoprofile) test, which measures the size of the LDL particles (LDL-P), which is thought to be more predictive of your cardiovascular risk, even if you have low total cholesterol2
- Oxidized LDL (oxLDL) test, which measures the level of LDLs that have been damaged by oxidation
- The apolipoprotein B (apoB) test, which measures the number of apoB particles in your blood. ApoB is a protein involved in the metabolism of lipids and the primary carrier for LDL. This test is a good predictor of cardiovascular risk, and does so far more accurately than the standard cholesterol panel
- Advanced lipid testing, which measures the amounts of large-buoyant LDLs (lbLDL) and small-dense LDLs (sdLDL), with the sdLDLs being associated with insulin resistance and heart disease3
High LDL Does Not Cause Atherosclerosis
When it comes to LDL cholesterol, the most important factor is the level of oxidized LDL, as oxLDLs are primarily what you find in atherosclerosis plaque.4 Unfortunately, most doctors will simply prescribe a statin drug or PCSK9 inhibitor if LDLs are high, to reduce the total LDL.
As noted by Ali in the short video above, this is a serious mistake. The primary question that needs to be asked is why is LDL oxidized in the first place, and how can you prevent that oxidation from taking place?
“Is the oxidized LDL a bad player?” Ali asks, “[or] is it there to protect us from oxidative injury? Rather than letting the important cells get oxidized, is the LDL sacrificing itself in protecting the body? Then, your whole paradigm changes …
LDL is not a bad player — it’s trying to protect us. What I need to figure out is how do I prevent this oxidative injury in the first place, and an argument that should surface is that, maybe I should have more LDL around so that oxidative injury can be … prevented, rather than having less LDL? These are the kinds of fundamental questions that science should be asking.”

Download this Article Before it Disappears
Oxidized LDL May Be a Protective Mechanism
Saladino agrees, saying that LDL “is probably a repository for oxidized phospholipids,” much like lipoprotein(a) (Lp(a)). He cites research showing that the more polyunsaturated fats (PUFAs) you consume — such as LA — the higher your Lp(a) and oxidized LDL.
So, your LDL may in fact have a protective rather than injurious role. It may protect you from the harmful effects of LA and other PUFAs. What this means, then, is that high oxidized LDL may be a marker of high PUFA consumption, and it’s the PUFAs, LA in particular, that are driving the atherosclerotic disease process.
The primary way to prevent atherosclerosis, then, is to radically reduce your LA intake by eliminating seed oils from your cooking, and avoiding processed foods (which are loaded with seed oils) and restaurant foods (as most are cooked in seed oils).
When it comes to measuring your oxLDL, the Boston Heart test called oxidized phospholipids on APO-B (OxPL/apoB) appears to be a better choice than the traditional oxLDL. The oxLDL tends to be inaccurate because it’s just a proxy for APO-B and the LDL number, while the OxPL/apoB test gives you a truer measure of your oxidized LDLs.
The ApoB Test
Aside from oxLDL, the apoB test can also be helpful in assessing your atherosclerosis risk. As mentioned above, apoB is the primary carrier for LDL, and research over the past decade shows it’s an accurate predictor of cardiovascular risk when apoB is high and LDL is normal. As reported by The Washington Post:5
“The standard cholesterol panel calculates the total quantity or concentration of ‘bad’ cholesterol or LDL in the blood, in milligrams per deciliter (technically, LDL-C). Because cholesterol is a fatty substance and thus not water-soluble, it must be carried around in little particles known as lipoproteins.
Testing for apoB, a protein on the outside of LDL-carrying particles, counts the number of these lipoprotein particles in the blood. In addition to LDL, it also captures other types of cholesterol such as IDL (intermediate-density lipoproteins) and VLDL (very low-density lipoproteins), which carry triglycerides.
Why is this important? As our understanding of heart disease improves, scientists are recognizing that apoB particles are more likely to become lodged in the arterial wall and cause it to thicken and eventually form atherosclerotic plaques. Thus, the total number of apoB particles matters more than the overall quantity of cholesterol that they carry.
In a majority of people, apoB and LDL-C track fairly closely, says Allan Sniderman, a professor of cardiology at McGill University in Montreal. But some people have a ‘normal’ amount of LDL-C, but a high concentration of apoB particles — a condition called ‘discordance,’ which means they are at greater risk.”
sdLDL — Another Helpful Predictor of Atherosclerosis
Measuring your sdLDL-C can also be helpful, as explained by Dr. Eric Berg, a chiropractor, in the video above. The small-dense type of LDLs are indicative of inflammation inside your arteries, which is a hallmark of atherosclerosis. As noted by Berg, potential causes of this inflammation include:
- Seed oils
- Processed foods and junk foods
- Smoking
- Low vitamin E
- High glucose levels
Unfortunately, Berg lumps high-carb diets into these risk factors and recommends a ketogenic diet to avoid elevated sdLDL, but as I’ve explained in previous articles, high glucose levels are not necessarily a sign that you’re eating too many (healthy) carbs.
In summary, when you consume significantly more than 30% fat, a metabolic switch called the Randle Cycle switches from burning glucose in your mitochondria to burning fat instead. As a result, glucose backs up into your bloodstream, thereby raising your blood sugar.
Glucose is actually a cleaner and far more efficient fuel than dietary fats, provided it’s metabolized in your mitochondria and not through glycolysis. For a refresher, refer back to “Crucial Facts About Your Metabolism” and “Important Information About Low Carb, Cortisol and Glucose.”
Atherosclerosis Is a Consequence of Metabolic Dysfunction
In the video directly above, Saladino debates LDL cholesterol with Dr. Mohammed Alo, a cardiologist and personal trainer. While Alo argues for the conventional LDL-atherosclerosis connection, Saladino highlights evidence showing that it’s not LDL per se that is the cause, but rather insulin resistance in combination with high oxLDL, both of which are caused by high LA intake.
For this reason, Saladino believes one of the best assessments of your heart disease risk is a fasting insulin test, as your insulin sensitivity is such a foundational factor of your metabolic function. The OxPL/apoB test mentioned earlier would be a good complement.
If you have high fasting insulin, you are insulin resistant and hence have some degree of metabolic dysfunction (and, of course, mitochondrial dysfunction). Ideally, you want a fasting insulin level of 3 mcg/mL or less.
Most definitely, do not go by the “normal” ranges offered by labs in this case. Many will list levels as high as 24 mcg/mL as normal, when in fact that’s a clear sign of serious insulin resistance and metabolic dysfunction.
If you’re already eating a healthy diet, exercising, and all of your metabolic parameters look good, yet you have an insulin level of 7 or 8, the core culprit may be stress, because when cortisol goes up, insulin rises with it. Cortisol release is a rescue mechanism to ensure you don’t die from low blood sugar.
To assess whether stress is at play, keep an eye on your white blood cell count. Chronically depleted white blood cells are often a sign of chronic stress and high cortisol.
You can also get an AM cortisol test after fasting for 12 to 16 hours. You don’t want to fast longer than that because, after 16 hours of fasting, cortisol will naturally start to rise. An ideal AM cortisol range is between 15 and 17. If your fasting AM cortisol is below 15, it’s a sign you’ve become stuck in a long-term stress response.
High LA Intake Promotes Atherosclerosis
So, to summarize, Saladino argues that insulin resistance is the primary root cause for atherosclerosis — not elevated LDL or total cholesterol — and the primary driver of insulin resistance is excessive LA intake from seed oils. Lowering your LA intake is the foundational strategy to embrace.6
Low levels of high-density lipoprotein (HDL) is a proxy for insulin resistance, and if you have low HDL, then LDL tracks well with cardiovascular disease. But if you have normal HDL (65 to 85 mg/dL), then you typically have good insulin sensitivity and the correlation with LDL and atherosclerosis vanishes.
The Keto Trial Match Analysis7 presented in mid-December 2023 (video below) confirms this, as they found no relationship between elevated LDL levels and arthrosclerosis plaque.
Other Tests to Assess Your Metabolic Health
In addition to the tests already mentioned, other blood tests that can help you assess your metabolic health include the following. Additional information about these and other lab tests can be found in my interviews with Dr. Nasha Winters and Dr. Bryan Walsh.
• Fasting glucose — The ideal range is between 82 and 88 milligrams per deciliter (mg/dL), based on the available literature, while nonfasting glucose should ideally be between 82 and 130 mg/dL.
• Gamma-glutamyl transferase (GGT), a powerful predictor of mortality, also should not be above 20 U/L. GGT is a liver enzyme involved in glutathione metabolism and the transport of amino acids and peptides.
Not only will the GGT test tell you if you have liver damage, it can also be used as a screening marker for excess free iron and is a great indicator of your sudden cardiac death risk.
GGT is highly interactive with iron. Excessive iron will tend to raise GGT, and when both your serum ferritin and GGT are high, you are at significantly increased risk of chronic health problems, because then you have a combination of free iron, which is highly toxic, and iron storage to keep that toxicity going.
Cysteinylglycine is liberated from glutathione via GGT. That, in the presence of iron or copper, initiates the Fenton reaction. That’s when you get massive oxidative stress.
• The Intermountain health risk score is a mortality risk score created based on the basic blood chemistry markers of tens of thousands of patients in a hospital setting, including complete blood count (CBC), sodium, potassium bicarbonate, mean platelet volume and other basics. Based on these markers, you end up with a 30-day, a one-year and a five-year mortality risk.
A risk score calculator is freely available on the Intermountain website, where you can also find more information about this score.8 Simply enter your variables and it will calculate your score for you.
• Coronary artery calcium (CAC) scan — This test provides images of your coronary arteries. Existing calcium deposits, an early sign of coronary artery disease, will show up on these images, and can therefore reveal your risk of heart disease before other warning signs become apparent.9
For even more information about cholesterol, and why high cholesterol and/or high LDL are not risk factors for heart disease, check out the video below by Dr. Ken Berry.
- 1 American Journal of Medicine May 1977; 62(5): 707-714
- 2 Front. Nuci. Med July 13, 2022; 2
- 3 Health Matters LDL Size
- 4 Mediators of Inflammation 2013; 2013: 714653
- 5 Washington Post January 8, 2024
- 6 Chem Phys Lipids January 1998; 91(1): 1-11
- 7 Citizens Science Foundation December 13, 2023
- 8 Intermountain Risk Scores
- 9 Hopkins Medicine CAC Test
How to Produce the Healthiest Foods Imaginable
Reproduced from original article:
https://articles.mercola.com/sites/articles/archive/2023/12/31/food-production.aspx
The original Mercola article may not remain on the original site, but I will endeavor to keep it on this site as long as I deem it to be appropriate.
Analysis by Dr. Joseph Mercola December 31, 2023
STORY AT-A-GLANCE
- Low-carb/high-fat diets ultimately backfire because they inhibit glucose metabolism, which is the most efficient form of energy production in the mitochondria; they also impair thyroid function
- One of the reasons why ketogenic and carnivore diets are usually helpful for a time is because, if implemented properly, you’re radically reducing your intake of omega-6 fats, linoleic acid (LA) in particular, which is one of the primary drivers of ill health
- LA is a primary driver of disease, in large part due to its detrimental effect on mitochondrial function and, hence, energy production
- Your body has a certain amount of energy and a number of biological processes that it can turn on or turn off with that energy pool. The more energy you have available, the more functions your body can turn on. When your energy production is lower than required to maintain all functions, your body must downregulate certain functions, which ultimately results in problems
- One of the easiest ways to assess how much energy your body is producing is to take your body temperature. Take your temperature 30 to 40 minutes after breakfast and midday. You want to see a rise in temperature
The interview above features Ashley Armstrong, who’s an expert in two areas. One is producing some of the healthiest food in the United States, and the second is understanding how your body uses it and how to select the right types of food to optimize your biology, based on the late biologist and thyroid expert, Ray Peat’s, principles of bioenergetic medicine. She also is a certified personal trainer with a Ph.D., MS and BS in engineering.
Like many others who are trying to improve their health, Armstrong tried low-carb diets, fasting, keto and even carnivore diets in the past. But while these all led to improvements initially, they didn’t eliminate them, which ultimately led her to investigate Peat’s principles.
“Ray Peat, he honestly saved my life and I owe so much to that man,” she says. “I’m forever grateful for him. The biggest wake-up for me was measuring my body temperature. I was on a carnivore diet and measured my body temperature — it was 96.5 degrees Fahrenheit.
I was like, wow, no wonder my hair is thinning. No wonder my complexion is so pale. No wonder I’m not sleeping through the night. There was just a number of red flags. That body temperature measurement just woke me up. It’s what I needed to [realize] I’m not thriving, I’m just surviving.
I’ve been implementing Dr. Peat’s principles for over three years now. I have more energy in life than I think I’ve ever had, even as a teenager. And it’s just amazing to see how being not restricted with your food, just being strategic with macros, types of food, how powerful that can be for your energy production.”
The Problem With Low-Carb and Keto
As I’ve detailed in previous articles over the past year, low-carb/high-fat diets ultimately backfire because they inhibit glucose metabolism, which is the most efficient form of energy production in your mitochondria; they also impair thyroid function. Your thyroid is crucial for energy production, and if your thyroid doesn’t work, you’re down the creek without a paddle.
One of the reasons for this is because ketogenic diets increase the stress hormones — cortisol, glucagon and adrenaline. On the other hand, one of the reasons why ketogenic and carnivore diets are usually helpful for a time is because, if implemented properly, you’re radically reducing your intake of omega-6 fats, linoleic acid (LA) in particular, which is one of the primary drivers of ill health.
Energy Production Is Key for Overall Health
As explained by Armstrong, the best way to understand the bioenergetic principle is to think of your body as a system. It has a certain amount of energy, and a number of biological processes that it can turn on or turn off with that energy source.
The greater your energy pool, the more functions your body can turn on. When your energy production is lower than required to maintain all functions, your body must downregulate certain functions, which ultimately results in problems. The human body is designed to promote survival, so it’s going to prioritize things like your heart rate.
Functions that aren’t necessarily vital for survival in the immediate moment, like sex hormone production, reproductive function, digestion, sleep and high cognitive thinking, get downregulated first. When you increase energy production, however, your body can then expend energy on those functions and bring them “back online.”

Download this Article Before it Disappears
Using Body and Pulse Measurements as Guides
As explained by Armstrong, one of the easiest ways to assess how much energy your body is producing is to take your body temperature.
“High stress hormones can keep your waking body temperature elevated,” she says, “so you’ve got to do your waking temperature 30 to 40 minutes after breakfast, and then I like to do midday. You want to see that temperature rise.
For many who are on low-carb or who are living on stress hormones, they’re going to have potentially high waking body temperature, but after breakfast, that temperature may drop. That’s because the food you’re consuming is lowering your stress hormones and your actual body temperature is then better exposed.
So we want to see that body temperature rise. And I love how both of us are so passionate about linoleic acid. As human linoleic acid consumption has gone up, human body temperature has gone down. So, the types of fats that we are consuming in our diet is impacting energy production in a negative way.
It’s shown with obesity rates out the roof. It’s shown with the decline in our body temperature. It’s shown with the decline in our healthy life expectancy, which is bizarre as a First-World country. There are just so many profound effects.
But when we just think of it as energy production — the more energy we can give our body to be able to perform functions, the better it’s going to function. I asked this question to someone who is really adamant about fasting. I said, ‘If you’ve got two bodies, one body that’s fasted and the other body that is fed nourishing food, which body is going to thrive and function better?’
It’s obvious. If you add a third person fed more of a standard American diet, of course maybe fasting is going to make you feel better, but you can elevate yourself a step above. You don’t have to rely on fasting to increase energy production. Your body is not going to increase energy when you’re not [putting] energy in.”
Indeed, when it comes to fasting, one of the primary benefits is that it lowers the fuel for gram-negative bacteria that produce endotoxin in your gut. Low-carb does this as well. Endotoxin, estrogen, LA and stress hormones will all decrease your mitochondrial function, mediated in big part by your thyroid function. Those are the big things that need to be reduced to enhance your mitochondrial function and energy production within the mitochondria.
How LA Harms Your Energy Production
As mentioned, LA is a primary driver of disease, in large part due to its detrimental effect on mitochondrial function and, hence, energy production. Your body can use both fat and glucose for energy. Muscle, in particular, will use fat for fuel, as will your heart. So, fat is not bad, but it’s important to realize that different fats affect your body in different ways, so it’s crucial to get the right fats. Armstrong explains:
“The different types of fatty acid molecules have drastically different structures and those impact the internal environment inside of us. They impact how your body is producing energy. The more saturated we can become, the better our internal environment is going to be.
When someone goes low-carb, maybe they reduce the amount of packaged food that they’re eating that contains a ton of vegetable oil and linoleic acid, and so potentially they’re resaturating some of their tissues.
But when you learn about what livestock are being fed these days, then you realize that a high animal fat diet can still contain quite a bit of PUFAs [polyunsaturated fats] and linoleic acid, depending on what those animals ate. So, think it’s important to consider the amount of each macronutrient that you’re intaking because that can have profound impacts on your energy production.
Saturating your tissues is going to take you to the next level, but adding in appropriate levels of carbohydrates is going to allow you to take your consciousness and energy production level to the next level [beyond that].”
The types of carbs you eat matter, however. I’m convinced the ideal carbohydrate is fresh, ripe fruit. Ripe is the key here. Of course, some fruits are better than others. Watermelon, for example, is among the best. Watermelon with feta cheese and a little mint on top makes for a delicious snack.
Aside from containing a lot of water, watermelon also contains a substance called citrulline, which converts into arginine, a precursor for nitric oxide (NO). NO is important to your body, but the caveat is that it needs to come from real food. Drugs like Cialis or Viagra, which act by increasing NO, will accelerate your path toward premature death. Artificial citrulline and other synthetic amino acids that raise NO are also best avoided.
“In Michigan, I rely a lot on frozen fruit,” Armstrong says. “In the summertime I’ll go to strawberry fields and pick strawberries when fresh and then freeze a ton of them. Same thing with blueberries and peaches. And then I rely on a lot of apples in the winter because apples are abundant around here and can be stored.”
Juices also have their place. Cold-pressed, pulp-free orange juice, for example, is a good choice. The reason you want pulp-free is because if you’re like most people, you have gram-negative, endotoxin bacteria in your gut that will thrive on the pulp, hence increasing endotoxin production.
So, if you have an unhealthy microbiome, pulp-free orange juice is a great carb that will gently and safely allow you to enter the higher carb world. As your microbiome improves, then you can transition to whole fruits and berries, which is, I believe, far superior to juices.
How to Produce the Best Eggs
Segueing into the topic of food production, Armstrong’s farm produces some of the highest quality eggs I’ve ever come across, and the feed recipe I use for my own chickens came from her. But I recently discovered something that could make them even better, and that is to allow the chickens to scratch for their own food.
Their ideal food is insects fresh from the ground, and while I previously thought chickens couldn’t get enough food this way, meaning you had to give them something, that may actually not be true.
Unfortunately, in places where the ground freezes, chickens will not be able to sustain themselves on insects, and you definitely do NOT want to feed your chickens dehydrated bugs. Why? Because the bugs are raised on corn and soy, making them very high in LA.
But in places like South Florida, for example, you can easily produce top-notch eggs, quality-wise, by allowing your chickens to peck for insects, without giving them any supplemental feed. Armstrong is also making plans to let her chickens forage for bugs year-round:
“I think that would be the ideal condition, and I have an image in my head of what I want to bring our farm to in the future — a greenhouse where we’ve got fodder growing on the ground and a worm farm … so [the chickens] will get abundant bugs in the winter. That’s what I want to move towards, but that requires a lot of financial investment. So we’ll get there one day.”
The Feed Has Dramatic Impacts on Animal Foods
The feed Armstrong developed, which I’ve been using as well, results in eggs that have about 75% less LA than conventional eggs. When it comes to conventional eggs, the LA is really the only problem. When the chickens are fed an ideal diet, the yolk in the egg is one of the best, most nutritious foods imaginable. The only thing that comes close is organ meat.
Egg yolks are the ultimate food; the problem is 99.99% of the eggs produced in this country are not that good. I don’t care if they say free range, grass fed, organic, it doesn’t matter. They’re terrible because they have four times more LA than they should. As noted by Armstrong:
“It’s important to consider organic soybeans have the same amount of linoleic acid as non-organic soybeans. Whether it’s grown conventionally, organically does not change the fatty acid composition of soybeans. You don’t want to be eating eggs from chickens fed a bunch of soy vegetable oil and other high omega-6 PUFA foods.”
According to Armstrong, the feed of the chickens may even determine the eggs’ allergenicity. In other words, if you’re allergic to eggs, you could potentially be able to eat the eggs from correctly-fed chickens.
“What is soy high in? Phytoestrogens that can be very problematic for some people. If a chicken is eating phytoestrogens that can be problematic for humans, those get passed through into the eggs. We have a number of customers that cannot eat any other eggs, but they’re totally fine with our eggs. And it’s because of the diet of the chicken.
So if you have allergic reactions or problems with eggs, try a different source where they’re not fed soy. Some people can be allergic to corn as well, and that allergenicity can pass through the egg as well. But it seems like soy is the biggest culprit.
But be careful of many corn and soy-free feeds, because those are high-PUFA ingredients like sunflower, flax, fish oil, vegetable oil and safflower oil. And so, just be really careful of your source, and ask what the chickens are eating. But yes, allergenicity of eggs I think really depends on what the chicken eats.”
LA-Rich Animal Feed Is Now Impacting Human Energy Production and Health
All of that said, it’s still crucial to ensure your chickens have enough food, be it fresh insects or a carefully planned feed that is low in LA and high in healthy saturated fats and other nutrients.
“Your chicken is not going to thrive if it’s underfed,” Armstrong says. “Your chicken is not going to thrive if it doesn’t have food. I am trying to boost the metabolic rate of our chickens as high as possible. Just like us, chickens are monogastric single stomach animals, the types of fat that they are fed, the types of fat that we are fed impacts the types of fat inside of us.
This is a little bit different for ruminant animals — cows, goats — but for monogastric chickens, pigs, their diet is very important. And this is why I am so passionate about it, because we have been lied to and convinced that saturated fat is bad for us.
So, you’ve seen a huge push for PUFAs in our diet. This is going beyond just human dietary choices. This is impacting our livestock food. And this is having profound impacts on not only livestock health, but also the food that we’re consuming …
Even in the dairy industry, they’re creating things called rumen-protected fats. They are PUFAs that in a typical rumen digestion system can go through the process called hydrogenation, which turns the PUFA into saturated fat.
They are designing rumen-protected fats so that the PUFA is passed through the rumen. The PUFA content of milk is increasing. That means any dairy fat — butter, cream, whole milk. The PUFA content of beef fat is increasing. And this is by design … Lard and chicken fat from conventional animals has the same amount of PUFA as canola oil.
This is profound. We have changed the types of fat inside of us. I think the linoleic acid content of humans has increased 136%. That is changing how our body is making energy inside of us. The types of fat we consume day-to-day have a long life inside of us — 600 days. So, the types of fat we’re consuming day to day impacts our energy production for years to come.
It’s unfortunate because this is just the reality for a lot of people, and that’s why I’m so passionate about it. Our food system is designed in a way that is not setting us up for success. That’s why I want to try to change it by going back to how our food was produced 100 years ago, where there was appropriate amounts of PUFAs in foods, small amounts, and saturated fat was the predominant fat source for both livestock and humans.”
High PUFA Diets Shut Down Your Metabolism
As explained by Armstrong, in nature, animals increase their PUFA consumption up to a certain amount to initiate torpor, which means their metabolism is so downregulated that they can survive the winter without eating. Think about that. Can you function optimally if your diet is one meant for hibernation? In that state, you have to eat fewer and fewer calories to avoid weight gain, which results in undernourishment and poor energy production.
“I try to keep my PUFA consumption as low as possible,” Armstrong says. “You can easily track that in Cronometer and see what your total PUFA, total linoleic acid content is per day. If you have four conventional eggs, you’re already at about 5 grams of linoleic acid in a day. And I would want people to be lower than that. All foods contain some amount of linoleic acid, so even milk is going to have a little bit.”
There’s no question that LA is NOT an essential fat, even though it’s categorized as such. It’s not essential because nearly all foods contain it. It’s virtually impossible to become deficient in LA if you eat food, regardless of what that food is.
Another fat that likely IS essential, but isn’t widely recognized as such, is the odd-chain saturated fats (OCFAs) found primarily in dairy. You can learn more about this in “The Amazing Benefits of Dairy Fat.” There’s also evidence suggesting that if you don’t get enough OCFAs in your diet, then high saturated fat intake might become problematic.
So, you need these odd-chain saturated fats. That’s why you need butter. You need milk. These are essential. Your optimized biology and health is dependent on these foods, because, again, the OCFAs help increase your body’s energy pool. They boost energy production, which will improve how your entire body functions.
In the interview we also discuss how dairy improves the health benefits of eggs, as the calcium in the dairy reduces the conversion of tryptophan in the egg white into serotonin. Serotonin is another compound you simply do not want too much of.
You also want to make sure you’re having enough carbohydrates with that meal. Carbohydrate oxidation produces 50% more carbon dioxide (CO2), so simply having carbs with your eggs will raise your CO2 level, which is very important for health.
“So, for breakfast, have eggs, milk, some honey or maple syrup and fruit. Boom, there you go. You’re drastically reducing the conversion of tryptophan to serotonin and it’s a simple meal,” Armstrong says.
More Information
We discuss a lot more in this interview than what I’ve covered here, so for more fascinating details, be sure to listen to the whole interview. For example, we discuss the pros and cons of egg whites, and why most cheese sold in the U.S. is less than healthy, as many cheese producers are using a microbial rennet made by Pfizer that is derived from mold that eats genetically modified corn and soy.
We also discuss various ideas for improving the feed of chickens, and how to maintain maximum egg production in the winter with incandescent lights and red light therapy.
If you want to purchase eggs from Armstrong’s farm, Angel Acres Egg Co., visit angel-acresfarm.com. She’s also started a new private member food system that offers milk, cheese, low-PUFA pork and low-PUFA chicken, called Nourish Cooperative. Both will ship farm-fresh food right to your door.
Vitamins A, B, C, D, E — What About Vitamin F?
Reproduced from original article:
https://articles.mercola.com/sites/articles/archive/2024/01/01/vitamin-f.aspx
The original Mercola article may not remain on the original site, but I will endeavor to keep it on this site as long as I deem it to be appropriate.
Analysis by Dr. Joseph Mercola January 01, 2024

STORY AT-A-GLANCE
- In the early 20th century, Casimir Funk, a Polish chemist, came up with the term “vitamine” — a compound that contains “amine,” which is Latin for nitrogen
- After Funk discovered vitamines, nutrition scientist Elmer McCollum revealed an “accessory” substance in certain fats that was needed for rats to grow; this substance was called vitamin A, for accessory
- McCollum and others named a nutrient vitamin B, for beriberi, while the different B vitamins were eventually numbered in the order they were discovered
- Vitamins were then named alphabetically until vitamin E; next came vitamin K, which is necessary for blood coagulation — or koagulation, as it was written in a German journal; rather than naming it vitamin F, the K abbreviation stuck
- Vitamin F did end up making a comeback, as it was used to name the essential fatty acids (EFAs) alpha-linolenic acid (ALA) and linoleic acid (LA)
Have you ever wondered what happened to vitamin F? We have vitamins A through E, and vitamin K, but vitamin F seems long forgotten. Getting to the bottom of the mystery requires digging into the history of vitamins, including how they came to be and the strategies used in naming them.
While it’s easy to take the knowledge of water- and fat-soluble vitamins for granted, it wasn’t until 1912 that the idea of vitamins came to be, setting the stage for more in-depth studies into these important nutritional compounds.
Nutrition Discoveries Came Before Vitamins
Humans have long had intrinsic knowledge that the foods they eat are tied to their health. In 1772, the discovery of nitrogen led to experiments on the element in food, followed by the discovery of an “animal substance” called protein in 1839. National Geographic reported:1
“For decades, historian Kenneth Carpenter writes, protein was considered the sole nutrient for human health despite emerging knowledge that fruits, vegetables, and milk eased conditions like scurvy and rickets. While these afflictions were common among those with limited diets, researchers still blamed other factors, like infections, tainted food, or even sea air.”
Around this time, it was recognized that beriberi, a disease now known to be caused by a vitamin B1 (thiamine) deficiency, may have a dietary link. Not only were poor people more likely to suffer from it than wealthier people, but those in prison who were fed white rice often developed the condition.
In the early 20th century, Casimir Funk, a Polish chemist, soon began to conduct experiments on pigeons, which revealed that those fed white rice grew ill. Their condition was reversed, however, when they ate rice bran and yeast. He suggested a “vitamine” — a compound that contains “amine,” which is Latin for nitrogen — was missing in the white rice diet, causing the pigeons to become sick. National Geographic continued:2
“The discovery of vitamins sent a shockwave through the scientific community, suggesting that diseases might be caused by nutritional deficiencies — and cured by adequate amounts of the newly discovered compounds. ‘A monotonous diet ought to be avoided,’ Funk declared. Researchers rushed to isolate other micronutrients associated with diseases like rickets, scurvy, goiters, and more.”
Vitamins Were Named Alphabetically — Until This
After Funk discovered vitamines, nutrition scientist Elmer McCollum revealed an “accessory” substance in certain fats that was needed for rats to grow. This substance was called vitamin A, for accessory. From there, McCollum and others named Funk’s rice bran nutrient vitamin B, for beriberi, while the different B vitamins were eventually numbered in the order they were discovered. As National Geographic noted:3
“The ‘e’ used in Funk’s new term was eventually dropped after scientists recognized that not all the compounds were nitrogen-containing amines. But the custom of naming vitamins alphabetically in order of discovery continued.
Today, four fat-soluble vitamins (A, D, E, and K) and nine water-soluble vitamins (Vitamin C and the eight B vitamins—B1 [thiamin], B2 [riboflavin], B3 [niacin], B5 [pantothenic acid], B6 [pyridoxine], B7 [biotin], B9 [folate], and B12 [cobalamin] — are considered essential to human growth and health.”
After vitamin E was discovered, Carl Peter Henrik Dam, a Danish biochemist, bucked the system with vitamin K, which is necessary for blood coagulation — or koagulation, as it was written in a German journal in which his research was published. Rather than naming it vitamin F, the K abbreviation stuck.

Download this Article Before it Disappears
Essential Fatty Acids Are Sometimes Called Vitamin F
Vitamin F did end up making a comeback, as it was used to name the essential fatty acids (EFAs) alpha-linolenic acid (ALA) and linoleic acid (LA).4 However, EFAs are need in substantial amounts, not trace amounts, which meant they didn’t meet the criteria to be called vitamins. For the record, Britannica defines vitamins as “any of several organic substances that are necessary in small quantities for normal health and growth in higher forms of animal life.”5
“Scientists discovered ALA and LA in the 1920s and mistook them for a vitamin they called vitamin F. The label stuck even though they were later found to be fats,” Cleveland Clinic reported.6 As explained by Nils Hoem, Ph.D., — a research scientist with Aker Biomarine, the largest krill oil company in the world — the plant-based omega-3 fats ALA and LA are both polyunsaturated fats (PUFAs) that are considered essential in conventional medicine.7
However, the amount of LA that many people consume in ultraprocessed foods has increased dramatically since its discovery. History shows that our lopsided consumption of ALAs began in the early 1900s, when people were discouraged from eating natural animal fats such as butter and lard.8 This led to a significant increase — more than two-fold — in the intake of LA, largely from vegetable oils.9
LA is an 18-carbon molecule. ALA also has 18 carbons. Since your body cannot make these fats, you must get them from your diet. That said, since LA is found in nearly every food, it’s virtually impossible to become deficient in LA. In fact, most people consume far too much LA, as it’s abundant in most ultraprocessed foods.
Others, such as the omega-3s EPA and DHA, which have 20 and 22 carbons respectively, can be synthesized in your body, provided you have enough available delta-6-desaturase, an enzyme responsible for their conversion.
The problem is that there’s competitive inhibition for that enzyme, so when you have 10-fold (1,000%) more omega-6 in your system, as many people do, then the delta-6-desaturase will be used to convert the omega-6 into arachidonic acid, instead of converting the ALA into EPA.
Since processed foods are loaded with omega-6 fats, it radically skews the omega-3 to omega-6 ratio and inhibits your body’s innate ability to synthesize beneficial EPA and DHA. Again, when you have large quantities of LA in your diet, it inhibits the enzyme, delta-6 desaturase, that converts ALA into EPA and then DHA.
So, it’s important to lower your LA intake as much as possible so your body can more easily convert any plant-based omega-3, found in flax, hemp and chia seeds, into the animal-based omega-3 fats EPA and DHA.
This competition for delta-6 becomes a moot point if you reduce your LA intake to only 1% to 2% of daily calories. But most people consume 20% to 25% of their calories in the form of LA, which means they have stored up this fat in their cells.
Restricting LA intake will balance out your omega-3s naturally, but increasing your intake of animal-based omega-3s is also important, as it can essentially push the omega-6 out of your membranes.
What About Vitamins G, H, I and J?
Other compounds once held the titles of the now-defunct vitamins G, H and J, although it seems I didn’t make the cut. According to The Globe and Mail:10
“Vitamin G is an obsolete name for riboflavin (now B2). H was the original name for biotin (now B7). There is no record of a historical vitamin I. Vitamin J has been associated with either riboflavin or the non-essential substance catechol, and M is an obsolete name for folic acid (B9).
Substances formerly referred to as vitamins L (anthranilic acid), N (thioctic or alpha-lipoic acid), O (carnitine), and P (flavonoids) are other examples of nutrients that do not meet the modern definition of a vitamin.”
More recently, vitamin G has been used to stand for “green space,” which is closely linked to physical and mental health and longevity.11
Vitamin Deficiencies Are Common
Despite widespread knowledge about the importance of vitamins for human health, many people are lacking in a variety of these compounds. Even at a subclinical level, being deficient in vitamins and minerals can cause a range of symptoms, ranging from fatigue and irritability to heart palpitations and pain.12 Common vitamin deficiencies include:
1. Vitamin D — Despite its name, vitamin D is not a regular vitamin. It’s a steroid hormone that your body is designed to obtain primarily through sun exposure, not via your diet. Worldwide, about 1 billion people are deficient in vitamin D, while an estimated 50% have vitamin D insufficiency.13
Older Americans tend to have the highest levels of vitamin D deficiency. In the U.S., 61% of older adults are deficient, rising to 90% in Turkey and 96% in India.14 In 2014, however, older Americans were already so deficient in vitamin D that it was estimated that as many as 100% of them were deficient, in large part due to less time spent outdoors.15
Vitamin D is necessary not only for healthy bones but for health throughout the body. As a powerful epigenetic regulator, vitamin D influences that activity of more than 2,500 genes, and vitamin D receptors are present all over the body, including in the intestine, pancreas, prostate and immune system cells.16 As noted in a systematic review published in Frontiers in Nutrition:17
“Previous association studies reported that vitamin D deficiency is also an important risk factor for SARS-CoV-2, weak muscle strength, cardiovascular disease, multiple sclerosis, upper respiratory tract infection, certain cancers, and other disease. In turn, these complications may increase the burden of global disease. Therefore, preventing vitamin D deficiency is a very important and urgent public health issue.”
I’ve long recommended a vitamin D level of 60 to 80 ng/ml (150-200 nmol/L) for optimal health and disease prevention. A level upward of 100 ng/mL also appears safe and beneficial for certain conditions, especially cancer.
However, the only way to gauge whether you might need to supplement, and how much to take, is to get your level tested, ideally twice a year, in the early spring, after the winter, and early fall when your level is at its peak and low point. Vitamin D is best obtained via sensible sun exposure, but supplementation may be necessary for some people.
2. Vitamin K2 — Known for its role in bone and heart health, vitamin K2 is found in grass fed animal products such as meat, eggs, liver and dairy,18 as well as in fermented foods, including sauerkraut, certain cheeses and the fermented soy food natto — items that many Americans do not consume enough of.
Vitamin K2, menaquinone, which is synthesized by intestinal bacteria, works synergistically with calcium, magnesium and vitamin D to build strong, healthy bone. Vitamin K2 directs calcium to your bones and prevents it from being deposited in your soft tissues, organs and joint spaces. Vitamin K2 also activates the protein hormone osteocalcin, produced by osteoblasts, which is needed to bind calcium into the matrix of your bone.
3. Vitamin B12 — A water-soluble vitamin also known as cobalamin, vitamin B12 plays a role in numerous biochemical reactions and neurological functions in your body, including DNA synthesis.19 Your body can’t make vitamin B12 on its own, so it must be obtained via your diet or supplementation.
It’s been suggested that nearly two-fifths of Americans may have lower than ideal B12 levels, with 9% deficient and 16% below 185 pmol/L, which is considered marginally deficient.20 While vegetarians and vegans are susceptible since B12 is derived from animal products, even meat eaters may be deficient, as problems with absorption are common.
4. Vitamin A — An estimated 51% of adults are not consuming enough vitamin A,21 increasing their risk of degenerative diseases like macular degeneration, a leading cause of blindness in the U.S.22
Vitamin A is a group of nutrients that falls into two different categories: retinoids found in animal foods and carotenoids found in plant foods. The two are chemically different and provide different health benefits, but both are necessary for optimal health. Plant foods high in beta-carotene include sweet potatoes, carrots, cantaloupe and mangoes.23 Animal foods rich in vitamin A include liver, egg yolks and grass fed butter.
If you think you may be missing out on important vitamins in your diet, the best way to boost your intake is via organic, whole foods. If you’re not eating right, a high-quality multivitamin may help fill in any gaps, with research suggesting they may improve biomarkers of nutrition compared to placebo.24,25
When choosing a multivitamin, be sure to look for a manufacturer that has checks and balances in place to ensure the quality of the product. And remember, since multivitamins contain both water- and fat-soluble vitamins, it’s generally recommended to take half your daily dose in the morning, with breakfast, and the other half with your main meal.
- 1, 2, 3 National Geographic November 9, 2023 (Archived)
- 4, 6 Cleveland Clinic, Vitamin F
- 5 Britannica, vitamin
- 7 Bitchute, Interview With Nils Hoem June 21, 2023
- 8, 9 BMJ Open Heart August 22, 2018
- 10 The Globe and Mail December 5, 2011
- 11 BMC Public Health. 2006; 6: 149
- 12 Nutrients. 2017 Jul; 9(7): 655
- 13, 14 National Library of Medicine, StatPearls, Vitamin D Deficiency, Epidemiology
- 15 J Aging Gerontol. 2014 Dec; 2(2): 60–71
- 16 Nutrients. 2021 Oct; 13(10): 3596. Intro
- 17 Frontiers in Nutrition March 17, 2023, Discussion
- 18 NIH. Vitamin K
- 19 Journal of Clinical Nephrology & Kidney Diseases August 31, 2018
- 20 USDA August 2000
- 21 Oregon State University, Micronutrient Inadequacies, Vitamin A
- 22 U.S. CDC, Macular Degeneration
- 23 National Institutes of Health, Vitamin A, Sources Of Vitamin A, Table 2
- 24 Oregon State University June 14, 2023
- 25 Nutrients 2023, 15(12), 2691; doi: 10.3390/nu15122691
Two Common Mistakes Athletes Make
STORY AT-A-GLANCE
- Runners can jeopardize their life by drinking too much water during a long-distance event. An estimated 10% to 20% of people have inappropriate secretion of antidiuretic hormone and retain fluid even though they’re overhydrated. As a result, they can lose consciousness and may die unless treated with concentrated salt solutions
- The treatment for overhydration is to give a high-saline IV (3% to 5% sodium). The sodium will absorb and help expel the excess water through urination, typically resulting in rapid recovery
- For non-athletes who are metabolically inflexible and have insulin resistance, a low-carb diet can help you regain your metabolic flexibility
- Dr. Mercola believes that once you’ve regained your metabolic flexibility, scientific evidence suggests a diet higher in carbs (primarily from ripe fruit) and restricting fat to about 30% of calories can optimize energy production and minimize harmful reactive oxygen species (ROS) production
In this interview, Timothy Noakes, Ph.D., a physician and sports medicine researcher in South Africa, clarifies common confusions about sports hydration and high-carb diets.
Noakes graduated from medical school in Cape Town, South Africa, in 1974, and received his research degree a few years later. Since then, he’s published more than 750 papers and a number of books, including the groundbreaking, “Waterlogged: The Serious Problem of Overhydration in Endurance Sports.”
“Waterlogged” countered the conventional view that you should drink as much as you can, even before you feel thirsty, to optimize your hydration. As it turns out, that can be dangerous advice for endurance athletes.
Overhydration Can Be Deadly
In early 1981, Noakes wrote an article arguing that runners must drink as much as they possibly can tolerate when running. “I’d been pushing that story for about 10 years,” he says.
A few months later, he received a letter from a woman who’d competed in the Comrades Marathon, a 56-mile South African ultramarathon. Some 40 miles into the race, she started losing her cognitive faculties and her husband took her to a medical facility.
Doctors declared that she was dehydrated and gave her 2 liters of intravenous normal saline (0.9% NaCl), at which point she lost consciousness and had an epileptic seizure. Her blood sodium was 112 units, well below the normal 140. Had she been given more dilute saline at this point, she may have died. Fortunately, the attending doctor restricted fluids and just waited. It took four days for her to regain consciousness.
“She’d been told she’d lost a lot of salt … and that this was the problem. I said to her, ‘Well, I have no idea, because this is the first case ever reported.’ But obviously, I was interested to find out [more]. So, I started phoning around and studying it.
Turned out there was another athlete who’d suffered a similar problem in the same race. And then I found another two cases. So, by 1985, I had four cases and it was clear to me that all had drunk too much fluid during the race …
The reason is because as the blood sodium concentration drops, the fluid expands the brain, and so the brain volume starts to increase. Ultimately, the pressure rises, stopping the blood flowing in or flowing out. As a consequence, the part of the brain that controls breathing herniates through the base of skull, and then you stop breathing. So that’s the cause of death. You stop breathing.”
According to Noakes, the treatment for overhydration is to give a high-saline IV (3% to 5% NaCl). Your kidneys cannot hold that much sodium, so it’s released into your urine where it helps expel the excess water through urination. Basically, the sodium acts as a diuretic. People usually make a rapid recovery within minutes to hours with this treatment.
Why Some Are Prone to Dangerous Overhydration
Because of all this, Noakes reversed his position on hydration during marathons, and published a paper on the dangers of fluid overload in 1985. Alas, the sports drinks industry in the U.S. was taking off at that time, and American runners were told to drink as much as possible, so his advice was not well-received.
“I predicted that the first person who would die from this condition would be a female runner in an American race,” Noakes says, “and that’s exactly what happened. In 1993, a runner in a California marathon died after the race. And again, she finished the race, she was semi-conscious, and then she was treated and the treatment was wrong.
Ultimately, we were able to prove that the condition doesn’t occur in everyone who overdrinks. Most people who overdrink simply pass more urine … What happens in this condition is that they’ve got inappropriate hormone secretion, antidiuretic hormone, and they retain fluid even though they’re overhydrated …
I think it’s genetic, in the sense that you either have it or you don’t. I think about 10% to 20% of people have that condition, so that when they overdrink, the body doesn’t recognize it as being overhydrated. It still thinks it’s dehydrated …
They’re running along and not passing urine, so they think, ‘My gosh, I’m dehydrated, so I must drink more.’ And that fluid is retained because this hormone is so powerful at retaining water. Ultimately, the brain swells and they lose consciousness.
Provided you leave them alone or give them a solid high-sodium infusion, they’re fine, but if you give them a low-sodium infusion, you’re going to kill them. I was demonized for saying all this. Eventually I wrote ‘Waterlogged,’ which … describes the whole history of what happened and [why] you should just drink to thirst.”

Download this Article Before it Disappears
Prosecuted for Breaking With Dietary Convention
Noakes also broke with conventional nutritional advice when he started recommending a high-fat diet. One day, he read a book called “The New Atkins for the New You,” and realized his dietary advice was likely completely wrong.
He decided to try the Atkins diet, which is a high-fat, high-protein, low-carb diet, and “had spectacular results,” including reversing his Type 2 diabetes. He recounts what happened next.
“I joined Twitter and did this very famous tweet [about the benefits of a low-carb diet] which caused me to be charged by the medical profession in South Africa for unprofessional behavior.
I had to go to court for over four years. Eventually I won the case and proved that the low carbohydrate diet has plenty of evidence behind it. It’s not unscientific. It’s in fact the most scientifically studied diet in the world.
So I won that case … At the same time, I was asked to start helping some other people with research and we started delving deeper, doing studies that I hadn’t done before on low carbohydrate diets.
Essentially, we are on the cusp of proving that humans don’t need carbohydrates … but when you come from an athletic background, you can’t believe that. Well, we’ve taken it to the extreme and we’ve shown that athletes who eat a high-fat diet, their performance is perfect, it’s completely normal.
So, my opinion is that the dietary macronutrient composition — the amount of carbohydrate and amount of fat you’re eating — has no effect on your athletic performance with one exception.
But the reason you burn carbohydrate is very clear to me. You burn carbohydrates to regulate your blood glucose concentration. That’s the key element of metabolism — to regulate your blood glucose.”
It is interesting that as a long-distance runner, Noakes developed diabetes. I used to believe that cardio was the cure for diabetes. It is well-known now that this is simply not the case. Food choices are responsible for causing diabetes.
However, excess carbs and not enough fat are not the reason someone develops diabetes. It is interesting to note that in 1890, about 2.8 people per 100,000 had diabetes. Today that number is likely north of 30,000 if you include those with prediabetes. That is a more than 100,000 times increase in a little over 130 years.
Increases in sugar intake or carbs did not cause this. It was the introduction of seed oils that caused severe mitochondrial dysfunction, causing the body to burn fatty acids rather than glucose. While limiting carbs can help when one develops diabetes, the solution is to radically reduce seed oils and every milligram of processed foods.
Athletes Don’t Need Carbs, Research Shows
Noakes believes humans didn’t have the need to regulate blood glucose until more recently, because we evolved eating mostly high-fat, high-protein diets. “We didn’t have a need to regulate blood glucose concentration because we weren’t eating stuff that was raising it,” he says.
I have great respect for Noakes and he is a kind and wonderful human being, but I believe that he is seriously mistaken on this point. He is just as confused as I was a few years ago on this issue. While fats can clearly fuel endurance cardio participants, that is entirely different from understanding what the best and most optimal fuel is for the mitochondria.
Noakes believes that over the last 50 years or so, we started eating very large quantities of carbs, but because our biology isn’t designed to cope with all those carbs, the coping mechanism is to burn it as soon as it’s consumed to lower the blood glucose level.
Sadly, the data simply don’t support Noakes’ assertion. From 1935 to 2016, the percentage of calories from sugar in the American diet rose only marginally from 22.5% to 24%. That’s an increase of just 1.5 percentage points.
Meanwhile, the consumption of seed oil skyrocketed from around 7% of total calories, which is still three times the recommended daily allowance (RDA), to a staggering 29% — nearly one-third of the modern American diet. So, while sugar edged up slightly, seed oils experienced exponential growth over the same time. Noakes continues:
“That’s why, when we study athletes who are eating a high carbohydrate diet … you see they’re burning so much carbohydrate, but they’re burning it to get rid of it, not because they need to use it,” Noakes says.
“We are the first people in 100 years to show that fat-adapted athletes can burn fat at very high rates in high intensity exercise, to the point where you could run a two-hour marathon burning fat alone. That’s what the data suggests.
We haven’t had a person run a two-hour marathon on a high fat diet, but the amount of energy required by Elliot Kipchoge when he runs a sub-two-hour marathon, is about 80 kilojoules per minute. Fat can provide 76 kilojoules per minute at least.
So he could run that race just burning fat, which of course conflicts with everything we’re taught. So that’s where we’re at, at the moment, and I’m working vigorously on finalizing the documents which prove that humans don’t need carbohydrates for exercise.
They can do very well with a minimum amount of carbohydrate … all you need is just to maintain your blood glucose concentration. Your blood glucose concentration is under stress during exercise, because even if you’re fully fat adapted, you can’t quite generate enough glucose to maintain your blood glucose for more than about three or four hours.
So, ultimately, if you don’t have carbs and if you’re a low-carb athlete, after about four hours you run into trouble. We are testing that hypothesis. We want to determine the minimum amount of carbohydrates you need, much as we determine the minimum amount of fluids you need during exercise.”
Processed Food Is a Primary Driver of Ill Health
I also embraced low-carb early on, and wrote a best-selling book called “Fat for Fuel.” So, I really understand the concept. I’ve endorsed it and recommended it. And, while my current recommendations have changed somewhat, I still think there’s great value in low-carb, primarily because most Americans are metabolically inflexible and insulin resistant. If that applies to you, a low-carb diet can help you regain your metabolic flexibility.
That said, since I wrote “Fat for Fuel,” I’ve come across additional information that has forced me to reconsider the value of staying on a low-carb, high-fat diet long-term. The late Ray Peat, a pioneer of bioenergetic medicine, advocated a relatively high glucose diet, but with specific types or carbs.
It is important to have carbs that have fructose in them, as fructose is an important fuel with many beneficial effects if it is consumed in the form of whole foods. The best foods with fructose are fruits and honey. Conversely, starches are long polymers of glucose with virtually no fructose.
Starches like white rice and white or red potatoes can be safely consumed if well-cooked, but most other starches are not digested in your small intestine, but travel to your large intestine where they are digested and form endotoxin, which is highly problematic for your health.
Curiously, evidence suggests both low-fat, high-carb, and high-fat, low-carb diets work equally well for Type 2 diabetes, but this would be extraordinary extremes, as health blogger Denise Minger points out in a lecture I plan to post soon.
I suspect the reason for that is because both diets tend to be whole food-based, so it’s really the avoidance of processed food that makes the biggest difference, and the single most destructive ingredient in processed food, based on my current understanding, is the omega-6 fat linoleic acid (LA).
So, to be clear, what Noakes is finding is that you don’t need carbohydrates to compete effectively in endurance events. I think that’s probably true, but the reason I went into medicine was because I have a passion to be healthy and to live as long as I can and teach others how to do that. And for a healthy life span, I now believe that optimizing glucose metabolism in your mitochondria is the key.
Glucose Appears To Be an Optimal Fuel for Health
Up until recently, I was convinced that fat was the ideal fuel to burn as a substrate in your mitochondria, but Peat’s work suggests that’s not true. What’s more, while you could technically survive without carbohydrates, because your body can make glucose from other substrates, that comes at a significant price.
The supposition is that to optimize longevity, you must optimize mitochondrial efficiency, and to do that, you want to burn the fuel that creates the most ATP and the least amount of ROS. If you have forward electron flow in the mitochondria, you can get to 99.9% efficiency.
Reductive stress facilitates reversal electron flow in the mitochondria, which raises ROS generation 30 to 40 times, and one of the things that contributes to reductive stress is beta oxidation of fat.
When beta oxidation occurs, the electrons don’t jump to Complex 1 in the electron transport chain; they jump to Complex 2, which contributes to reductive stress. And, while LA is the worst culprit, causing the greatest amount of reductive stress, even healthy saturated fats will have this effect.
In addition to creating far less ROS, burning glucose in your mitochondria will also generate far more carbon dioxide and metabolic water, as opposed to creating lactate when it is burned in glycolysis.
What’s more, when your glucose level gets too low, you’re going to secrete cortisol. Cortisol creates glucose by stripping amino acids from your bones, brain and muscles. So, the danger of going low-carb long-term is that you can end up with chronically elevated cortisol, which leads to a lot of complications, including sarcopenia (muscle loss).
I believe Noakes’ observation may be related to the fact he was working with cardiac cells, which are an exception to most tissues in your body, as at rest, heart cells are designed to burn fat, not sugar. Noakes comments:
“The focus for my Ph.D. was, what was the fuel that made the heart perform the best? And I came to the conclusion that glucose and insulin were actually the optimum, but the very first experiment I did was to add ketones to glucose and the heart functioned a lot better.
I left it at that and didn’t deal with it any further, unfortunately, because Richard Veech did exactly the same experiments 10 years or so later, and came to the conclusion that ketone metabolism was crucial for whole body metabolism.
If I read the introduction to his article, therapeutic potentials of mild ketosis flow directly from a thorough understanding of their metabolic effects, particularly upon mitochondrial redox states, energetics and substrate availability …
There’s a lovely book, ‘Ketones, the Fourth Fuel,’ written by Travis Christofferson, in which he talks about [Otto] Warburg … Hans Krebs [and] Veech … They were the three people who really promoted ketone metabolism and its understanding.
So I’m not the authority, but it seems to me that ketones do have a special role in mitochondrial metabolism, and do exactly what you’re suggesting the carbohydrates do …
Veech came up to the conclusion that ketones had a special role in minimizing mitochondrial electron overflow, as you suggested, and oxidative stress. But I haven’t really studied closely enough all his research …”
How Much Fat Is Too Much?
An expert in the Randle cycle, Noakes agrees that high amounts of fat inhibit glucose metabolism, which is why you cannot simply add more carbs if you’re eating high amounts of fat. Your body simply won’t be able to burn those extra carbs for fuel.
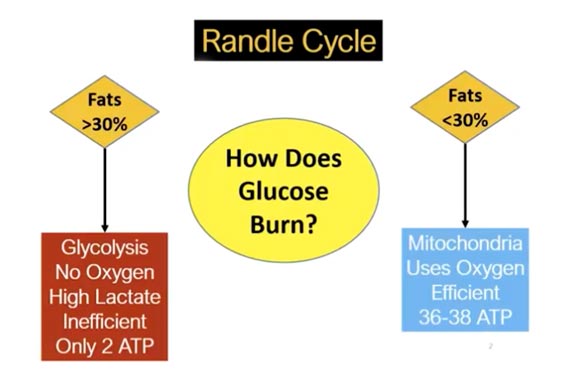
The Randle cycle is going to inhibit the oxidation of glucose in the mitochondria, resulting in weight gain, reduced energy production and other problems. If you’re metabolically impaired, as most people are, your fat intake may need to be as low as 10% to 15% initially, to prevent glycolysis from occurring.
Over time, you can then raise your fat intake to about 30% and still maintain healthy glucose metabolism. Unless you minimize your LA intake and get your total fat content below 30%, you really can’t go high-carb, because the end result is predictable. It’ll lead to diabetes, especially you have high tissue levels of LA, because the glucose cannot be metabolized in your mitochondria and will go to glycolysis instead.
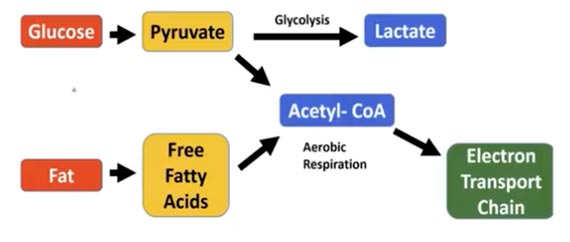
You also cannot load in just any type of carbohydrates. Most grains are loaded with LA and are therefore best avoided. Resistant starches also need to be limited, as they fuel the production of endotoxins in your gut.
The best carbs are ripe fruits. In addition to being a source of carbohydrates, ripe fruits also contain high levels of potassium, which will balance your sodium. Other healthy carbs include white rice and well-cooked potatoes.
Noakes’ Model: Muscle Glycogen Determines Fat Metabolism
Interestingly, in 1999, Noakes did a study showing that it’s not the Randle cycle that determines fat metabolism but, rather, the muscle glycogen content. In other words, the amount of glycogen in your muscles determines how much fat you burn. He explains:
“We made people glycogen depleted, and then we infused glucose. The glucose infusion made no difference. They refused to burn the extra glucose because they were burning so much fat when the glycogen was low.
In fact, I found an old paper [showing] that the best way to normalize your glucose tolerance is to get your muscle glycogen to zero, or as low as possible, and that fits my model.
My model is that when you take carbohydrate, the first thing you do is you try to burn it, so you inhibit fat oxidation, and then you dump it into muscle … and then you’ve got to exercise, get rid of it, and you cannot stop muscle glycogen burning. You cannot.
You can do what you like, it doesn’t stop muscle glycogen use. So, you can infuse glucose at high rates, the muscles will still burn the glycogen. If there’s glycogen in the muscle, it will be burned. And you have to ask why, when there’s so much fat to be oxidized?
So that’s the model that I see. I see the human as being loving to burn fat, and we’ve destroyed that by feeding them linoleic acid and carbs for too long. That’s how I see it.”
Why Strength Training Is so Important
Importantly, muscle glycogen is only used in the muscle. The glycogen cannot be excreted or secreted into your bloodstream. Only glycogen in the liver can do that. This makes a strong case for resistance training and building significant muscle mass. Like me, Noakes switched from running to doing resistance training when he got older:
“I’ve also shifted to weights and resistance training and it’s astonishing. When I look back, the benefits I get as a 74-year-old from resistance training are equal to the benefits I used to get at running as a 20 year old or a 30 year old. Today I can’t get those benefits from running anymore.
You have to change. And I’ve met a lot of endurance athletes who’ve told me that once they crossed 60, they reduced the running or the cycling and moved into resistance training, with huge benefits.”
Life Requires Constant Adaptation
In conclusion, Noakes correctly (and humbly) admits that when it comes to diet and exercise, we cannot make absolute statements that will be correct and always apply to everyone. We have an obligation to experiment and discover what works best for us, in the moment, and realize that what was best a few years ago may no longer be ideal.
To give you a personal example, when I shifted over from high-fat, low-carb to relatively high-carb, low-fat (upping my carbs from 150 grams a day to 400 or 500 grams) I lost 10 pounds, my body fat decreased 3% and my fasting blood sugar went down 10 points.
So, my body was telling me, “This is something I want to do.” It was clear that, from a blood work perspective and biological parameters, I was moving in the right direction. That intrigued me, because I like to test these theories out on myself before I start espousing them to others.
Before that, I was convinced that long-term high fat, low carb dieting was the way to go. My experience told me I hadn’t completely nailed it and needed to refine my recommendations further, which is why I’m now presenting more information about the benefits of higher-carb, lower-fat diets.
The caveat is that you need to be mindful of the types of carbs you add in, and to avoid seed oils. Unless you lower the LA, high-carb is not going to be a good strategy. Also, if you’re not exercising enough, eating 500 grams of carbs is going to be a disaster.
To learn more about Noakes’ work, please visit thenoakesfoundation.org. Also consider sponsoring his research efforts by making a donation, or become a research participant by filling out an anecdotal data collection form.